Key Points
-
Most of our understanding of memory T cell generation, function and maintenance comes from mouse studies, which cannot recapitulate the exposure to diverse antigens and microbiota that occurs over many decades in humans.
-
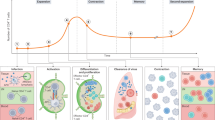
Memory T cell frequency dynamically changes throughout the human lifetime and this can be divided into three phases: memory generation, memory homeostasis and immunosenescence.
-
CD45RO+CD45RA− T cells comprise diverse memory T cell subsets, including central memory T (TCM) cells, effector memory T (TEM) cells, stem cell memory T (TSCM) cells and tissue-resident memory T (TRM) cells, which are heterogeneous in their generation, distribution and function.
-
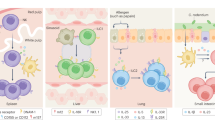
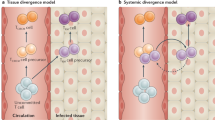
Memory T cells that are specific for antigens from ubiquitous pathogens and possibly from endogenous flora are generated early in life and are preferentially compartmentalized at the sites of infection throughout adulthood.
-
Human memory T cells in diverse tissue sites are homeostatically maintained, potentially through tonic T cell receptor signalling, and can show extensive cross reactivity and can persist for decades.
-
The induction of memory CD4+ and CD8+ T cells through vaccination can enhance protection against pathogens, and might be improved by considering the anatomical location and the timing of vaccine administration during the early stages of life.
Abstract
Memory T cells constitute the most abundant lymphocyte population in the body for the majority of a person's lifetime; however, our understanding of memory T cell generation, function and maintenance mainly derives from mouse studies, which cannot recapitulate the exposure to multiple pathogens that occurs over many decades in humans. In this Review, we discuss studies focused on human memory T cells that reveal key properties of these cells, including subset heterogeneity and diverse tissue residence in multiple mucosal and lymphoid tissue sites. We also review how the function and the adaptability of human memory T cells depend on spatial and temporal compartmentalization.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
References
Remakus, S. & Sigal, L. J. Memory CD8+ T cell protection. Adv. Exp. Med. Biol. 785, 77–86 (2013).
Wherry, E. J. & Ahmed, R. Memory CD8 T-cell differentiation during viral infection. J. Virol. 78, 5535–5545 (2004).
Teijaro, J. R. et al. Costimulation modulation uncouples protection from immunopathology in memory T cell responses to influenza virus. J. Immunol. 182, 6834–6843 (2009).
Teijaro, J. R. et al. Cutting edge: tissue-retentive lung memory CD4 T cells mediate optimal protection to respiratory virus infection. J. Immunol. 187, 5510–5514 (2011). This study identifies the retention of CD4+ T RM cells in mouse lungs and shows that lung T RM cells have a superior protective capacity against influenza virus infection compared with circulating spleen memory CD4+ T cells.
Teijaro, J. R., Verhoeven, D., Page, C. A., Turner, D. & Farber, D. L. Memory CD4 T cells direct protective responses to influenza virus in the lungs through helper-independent mechanisms. J. Virol. 84, 9217–9226 (2010).
Khader, S. A. et al. IL-23 and IL-17 in the establishment of protective pulmonary CD4+ T cell responses after vaccination and during Mycobacterium tuberculosis challenge. Nature Immunol. 8, 369–377 (2007).
Anthony, R. M. et al. Memory TH2 cells induce alternatively activated macrophages to mediate protection against nematode parasites. Nature Med. 12, 955–960 (2006).
McFall-Ngai, M. Adaptive immunity: care for the community. Nature 445, 153 (2007).
Cossarizza, A. et al. CD45 isoforms expression on CD4+ and CD8+ T cells throughout life, from newborns to centenarians: implications for T cell memory. Mech. Ageing Dev. 86, 173–195 (1996). This paper is an early survey of memory T cell frequencies in peripheral blood throughout the human lifespan.
Christensen, K. L. et al. Infectious disease hospitalizations in the United States. Clin. Infect. Dis. 49, 1025–1035 (2009).
Sathaliyawala, T. et al. Distribution and compartmentalization of human circulating and tissue-resident memory T cell subsets. Immunity 38, 187–197 (2013). This study describes a whole-body analysis of T cell subsets in the blood and in multiple lymphoid and mucosal sites from individual organ donors. It identifies how memory T cell subsets are differentially compartmentalized in tissue sites and that this compartmentalization is remarkably conserved between diverse individuals.
Saule, P. et al. Accumulation of memory T cells from childhood to old age: central and effector memory cells in CD4+ versus effector memory and terminally differentiated memory cells in CD8+ compartment. Mech. Ageing Dev. 127, 274–281 (2006). This paper is an excellent survey of peripheral blood T cell subsets in a large cohort of individuals from birth to old age.
den Braber, I. et al. Maintenance of peripheral naive T cells is sustained by thymus output in mice but not humans. Immunity 36, 288–297 (2012).
Goronzy, J. J. & Weyand, C. M. Understanding immunosenescence to improve responses to vaccines. Nature Immunol. 14, 428–436 (2013).
Nikolich-Zugich, J. & Rudd, B. D. Immune memory and aging: an infinite or finite resource? Curr. Opin. Immunol. 22, 535–540 (2010).
Clark, R. A. et al. The vast majority of CLA+ T cells are resident in normal skin. J. Immunol. 176, 4431–4439 (2006).
Clark, R. A. et al. A novel method for the isolation of skin resident T cells from normal and diseased human skin. J. Invest. Dermatol. 126, 1059–1070 (2006).
Purwar, R. et al. Resident memory T cells (TRM) are abundant in human lung: diversity, function, and antigen specificity. PLoS ONE. 6, e16245 (2011). The study describes the phenotype and the functional properties of human T RM cells in lung tissue.
Ganusov, V. V. & De Boer, R. J. Do most lymphocytes in humans really reside in the gut? Trends Immunol. 28, 514–518 (2007). This study provides a novel quantitative assessment of human T cell numbers in mucosal and lymphoid tissues.
Mueller, S. N., Gebhardt, T., Carbone, F. R. & Heath, W. R. Memory T cell subsets, migration patterns, and tissue residence. Annu. Rev. Immunol. 31, 137–161 (2013).
Bunders, M. J. et al. Memory CD4+CCR5+ T cells are abundantly present in the gut of newborn infants to facilitate mother-to-child transmission of HIV-1. Blood 120, 4383–4390 (2012).
Dos Santos, A. B. et al. Immune cell profile in infants' lung tissue. Ann. Anat. http://dx.doi.org/10.1016/j.aanat.2013.05.003 (2013).
Kupper, T. S. Old and new: recent innovations in vaccine biology and skin T cells. J. Invest. Dermatol. 132, 829–834 (2012).
Sanders, M. E. et al. Human memory T lymphocytes express increased levels of three cell adhesion molecules (LFA-3, CD2, and LFA-1) and three other molecules (UCHL1, CDw29, and Pgp-1) and have enhanced IFNγ production. J. Immunol. 140, 1401–1407 (1988).
Smith, S. H., Brown, M. H., Rowe, D., Callard, R. E. & Beverley, P. C. Functional subsets of human helper-inducer cells defined by a new monoclonal antibody, UCHL1. Immunology 58, 63–70 (1986).
Sallusto, F., Lenig, D., Forster, R., Lipp, M. & Lanzavecchia, A. Two subsets of memory T lymphocytes with distinct homing potentials and effector functions. Nature 401, 708–712 (1999). This publication is a seminal study that describes memory T cell heterogeneity in humans and establishes a new paradigm for memory T cell heterogeneity.
Sallusto, F., Geginat, J. & Lanzavecchia, A. Central memory and effector memory T cell subsets: function, generation, and maintenance. Annu. Rev. Immunol. 22, 745–763 (2004).
Masopust, D., Vezys, V., Marzo, A. L. & Lefrancois, L. Preferential localization of effector memory cells in nonlymphoid tissue. Science 291, 2413–2417 (2001). This study establishes the heterogeneous tissue distribution of antiviral memory CD8+ T cells, as well as the biased distribution of T EM cells in non-lymphoid sites.
Reinhardt, R. L., Khoruts, A., Merica, R., Zell, T. & Jenkins, M. K. Visualizing the generation of memory CD4 T cells in the whole body. Nature 410, 101–105 (2001).
Wang, A. et al. The stoichiometric production of IL-2 and IFNγ mRNA defines memory T cells that can self-renew after adoptive transfer in humans. Sci. Transl. Med. 4, 149ra120 (2012).
Pedron, B. et al. Development of cytomegalovirus and adenovirus-specific memory CD4 T-cell functions from birth to adulthood. Pediatr. Res. 69, 106–111 (2011). In this study, the authors provide a comprehensive assessment of CMV-specific and adenovirus-specific memory T cells in a large cohort, in cross-sectional studies of individuals from birth to throughout adulthood.
Champagne, P. et al. Skewed maturation of memory HIV-specific CD8 T lymphocytes. Nature 410, 106–111 (2001).
Ellefsen, K. et al. Distribution and functional analysis of memory antiviral CD8 T cell responses in HIV-1 and cytomegalovirus infections. Eur. J. Immunol. 32, 3756–3764 (2002).
Fearon, D. T., Carr, J. M., Telaranta, A., Carrasco, M. J. & Thaventhiran, J. E. The rationale for the IL-2-independent generation of the self-renewing central memory CD8+ T cells. Immunol. Rev. 211, 104–118 (2006).
Gattinoni, L. et al. A human memory T cell subset with stem cell-like properties. Nature Med. 17, 1290–1297 (2011). This study identifies a new, self-renewing population of memory T cells in human blood, designated T SCM cells, and provides functional and phenotypic characterization, as well as enumerating their potential in immunotherapy.
Zhang, Y., Joe, G., Hexner, E., Zhu, J. & Emerson, S. G. Host-reactive CD8+ memory stem cells in graft-versus-host disease. Nature Med. 11, 1299–1305 (2005).
Gattinoni, L., Ji, Y. & Restifo, N. P. Wnt/β-catenin signaling in T-cell immunity and cancer immunotherapy. Clin. Cancer Res. 16, 4695–4701 (2010).
Gattinoni, L., Klebanoff, C. A. & Restifo, N. P. Paths to stemness: building the ultimate antitumour T cell. Nature Rev. Cancer. 12, 671–684 (2012).
Klebanoff, C. A., Gattinoni, L. & Restifo, N. P. CD8+ T-cell memory in tumor immunology and immunotherapy. Immunol. Rev. 211, 214–224 (2006).
Lanzavecchia, A. & Sallusto, F. Progressive differentiation and selection of the fittest in the immune response. Nature Rev. Immunol. 2, 982–987 (2002).
Ahmed, R., Bevan, M. J., Reiner, S. L. & Fearon, D. T. The precursors of memory: models and controversies. Nature Rev. Immunol. 9, 662–668 (2009).
Buchholz, V. R. et al. Disparate individual fates compose robust CD8+ T cell immunity. Science 340, 630–635 (2013).
Gerlach, C. et al. Heterogeneous differentiation patterns of individual CD8+ T cells. Science 340, 635–639 (2013).
Stemberger, C. et al. A single naive CD8+ T cell precursor can develop into diverse effector and memory subsets. Immunity 27, 985–997 (2007).
Chang, J. T. et al. Asymmetric T lymphocyte division in the initiation of adaptive immune responses. Science 315, 1687–1691 (2007).
Campbell, J. J. et al. CCR7 expression and memory T cell diversity in humans. J. Immunol. 166, 877–884 (2001).
Turner, D. L. et al. Lung niches for the generation and maintenance of tissue-resident memory T cells. Mucosal Immunol. http://dx.doi.org/10.1038/mi.2013.67 (2013).
Herndler-Brandstetter, D. et al. Human bone marrow hosts polyfunctional memory CD4+ and CD8+ T cells with close contact to IL-15-producing cells. J. Immunol. 186, 6965–6971 (2011).
Klonowski, K. D. et al. Dynamics of blood-borne CD8 memory T cell migration in vivo. Immunity 20, 551–562 (2004).
Clark, R. A. et al. Skin effector memory T cells do not recirculate and provide immune protection in alemtuzumab-treated CTCL patients. Sci. Transl. Med. 4, 117ra117 (2012). By examining a cohort of patients being treated with T cell depletion therapy that reduces peripheral T cell numbers, this study provides evidence that T RM cells in the human skin can provide protection against virus infection.
Liu, L. et al. Epidermal injury and infection during poxvirus immunization is crucial for the generation of highly protective T cell-mediated immunity. Nature Med. 16, 224–227 (2010).
Mackay, L. K. et al. Long-lived epithelial immunity by tissue-resident memory T (TRM) cells in the absence of persisting local antigen presentation. Proc. Natl Acad. Sci. USA 109, 7037–7042 (2012).
Shin, H. & Iwasaki, A. A vaccine strategy that protects against genital herpes by establishing local memory T cells. Nature 491, 463–467 (2012).
Masopust, D. et al. Dynamic T cell migration program provides resident memory within intestinal epithelium. J. Exp. Med. 207, 553–564 (2010).
Masopust, D., Vezys, V., Wherry, E. J., Barber, D. L. & Ahmed, R. Cutting edge: gut microenvironment promotes differentiation of a unique memory CD8 T cell population. J. Immunol. 176, 2079–2083 (2006).
Anderson, K. G. et al. Cutting edge: intravascular staining redefines lung CD8 T cell responses. J. Immunol. 189, 2702–2706 (2012).
Wakim, L. M., Woodward-Davis, A. & Bevan, M. J. Memory T cells persisting within the brain after local infection show functional adaptations to their tissue of residence. Proc. Natl Acad. Sci. USA 107, 17872–17879 (2010).
Casey, K. A. et al. Antigen-independent differentiation and maintenance of effector-like resident memory T cells in tissues. J. Immunol. 188, 4866–4875 (2012).
Masopust, D. & Picker, L. J. Hidden memories: frontline memory T cells and early pathogen interception. J. Immunol. 188, 5811–5817 (2012).
Gebhardt, T. & Mackay, L. K. Local immunity by tissue-resident CD8+ memory T cells. Front. Immunol. 3, 340 (2012).
Jiang, X. et al. Skin infection generates non-migratory memory CD8+ TRM cells providing global skin immunity. Nature 483, 227–231 (2012). This study shows that, in mice, skin T RM cells do not circulate and that these cells mediate protection to viral infection of the skin.
Gebhardt, T. et al. Memory T cells in nonlymphoid tissue that provide enhanced local immunity during infection with herpes simplex virus. Nature Immunol. 10, 524–530 (2009).
Wakim, L. M., Gebhardt, T., Heath, W. R. & Carbone, F. R. Cutting edge: local recall responses by memory T cells newly recruited to peripheral nonlymphoid tissues. J. Immunol. 181, 5837–5841 (2008).
Tokoyoda, K. et al. Professional memory CD4+ T lymphocytes preferentially reside and rest in the bone marrow. Immunity 30, 721–730 (2009).
Lugli, E. et al. Superior T memory stem cell persistence supports long-lived T cell memory. J. Clin. Invest. 123, 594–599 (2013).
Gebhardt, T., Mueller, S. N., Heath, W. R. & Carbone, F. R. Peripheral tissue surveillance and residency by memory T cells. Trends Immunol. 34, 27–32 (2013).
Clark, R. A. Skin-resident T cells: the ups and downs of on site immunity. J. Invest. Dermatol. 130, 362–370 (2010).
Homey, B. et al. CCL27–CCR10 interactions regulate T cell-mediated skin inflammation. Nature Med. 8, 157–165 (2002).
Kunkel, E. J. et al. Lymphocyte CC-chemokine receptor 9 and epithelial thymus-expressed chemokine (TECK) expression distinguish the small intestinal immune compartment: Epithelial expression of tissue-specific chemokines as an organizing principle in regional immunity. J. Exp. Med. 192, 761–768 (2000).
Agace, W. W. T-cell recruitment to the intestinal mucosa. Trends Immunol. 29, 514–522 (2008).
Ruane, D. et al. Lung dendritic cells induce migration of protective T cells to the gastrointestinal tract. J. Exp. Med. 210, 1871–1888 (2013).
Edele, F. et al. Cutting edge: instructive role of peripheral tissue cells in the imprinting of T cell homing receptor patterns. J. Immunol. 181, 3745–3749 (2008).
Stagg, A. J., Kamm, M. A. & Knight, S. C. Intestinal dendritic cells increase T cell expression of α4β7 integrin. Eur. J. Immunol. 32, 1445–1454 (2002).
Cimbro, R. et al. IL-7 induces expression and activation of integrin α4β7 promoting naive T-cell homing to the intestinal mucosa. Blood 120, 2610–2619 (2012).
Zhang, H. H. et al. CCR2 identifies a stable population of human effector memory CD4+ T cells equipped for rapid recall response. J. Immunol. 185, 6646–6663 (2010).
Kim, C. H. et al. Rules of chemokine receptor association with T cell polarization in vivo. J. Clin. Invest. 108, 1331–1339 (2001).
Campbell, D. J., Kim, C. H. & Butcher, E. C. Chemokines in the systemic organization of immunity. Immunol. Rev. 195, 58–71 (2003).
Andrew, D. P. et al. CC chemokine receptor 4 expression defines a major subset of circulating nonintestinal memory T cells of both TH1 and TH2 potential. J. Immunol. 166, 103–111 (2001).
Seder, R. A., Darrah, P. A. & Roederer, M. T-cell quality in memory and protection: implications for vaccine design. Nature Rev. Immunol. 8, 247–258 (2008).
Zhang, X. et al. Human bone marrow: a reservoir for “enhanced effector memory” CD8+ T cells with potent recall function. J. Immunol. 177, 6730–6737 (2006).
Singh, S. P., Zhang, H. H., Foley, J. F., Hedrick, M. N. & Farber, J. M. Human T cells that are able to produce IL-17 express the chemokine receptor CCR6. J. Immunol. 180, 214–221 (2008). This study shows how IL-17-producing human memory T cells are specifically maintained within a CCR6-expressing T cell subset.
Wan, Q. et al. Cytokine signals through PI-3 kinase pathway modulate TH17 cytokine production by CCR6+ human memory T cells. J. Exp. Med. 208, 1875–1887 (2011).
Cosmi, L. et al. Human interleukin 17-producing cells originate from a CD161+CD4+ T cell precursor. J. Exp. Med. 205, 1903–1916 (2008). This study identifies a specific subset of IL-17-producing memory T cells that expresses CD161 in inflamed tissues.
Duhen, T., Geiger, R., Jarrossay, D., Lanzavecchia, A. & Sallusto, F. Production of interleukin 22 but not interleukin 17 by a subset of human skin-homing memory T cells. Nature Immunol. 10, 857–863 (2009).
Eyerich, S. et al. TH22 cells represent a distinct human T cell subset involved in epidermal immunity and remodeling. J. Clin. Invest. 119, 3573–3585 (2009).
Murali-Krishna, K. et al. Counting antigen-specific CD8 T cells: a reevaluation of bystander activation during viral infection. Immunity 8, 177–187 (1998).
Chomont, N., DaFonseca, S., Vandergeeten, C., Ancuta, P. & Sekaly, R. P. Maintenance of CD4+ T-cell memory and HIV persistence: keeping memory, keeping HIV. Curr. Opin. HIV AIDS 6, 30–36 (2011).
Chomont, N. et al. HIV reservoir size and persistence are driven by T cell survival and homeostatic proliferation. Nature Med. 15, 893–900 (2009).
Eisele, E. & Siliciano, R. F. Redefining the viral reservoirs that prevent HIV-1 eradication. Immunity 37, 377–388 (2012).
Chakrabarti, L. A. & Simon, V. Immune mechanisms of HIV control. Curr. Opin. Immunol. 22, 488–496 (2010).
Youngblood, B., Wherry, E. J. & Ahmed, R. Acquired transcriptional programming in functional and exhausted virus-specific CD8 T cells. Curr. Opin. HIV AIDS 7, 50–57 (2012).
Walker, B. & McMichael, A. The T-cell response to HIV. Cold Spring Harb Perspect Med. http://dx.doi.org/10.1101/cshperspect.a007054 (2012).
Marchant, A. et al. Mature CD8+ T lymphocyte response to viral infection during fetal life. J. Clin. Invest. 111, 1747–1755 (2003).
Komatsu, H. et al. Large scale analysis of pediatric antiviral CD8+ T cell populations reveals sustained, functional and mature responses. Immun. Ageing 3, 11 (2006).
He, X. S. et al. Cellular immune responses in children and adults receiving inactivated or live attenuated influenza vaccines. J. Virol. 80, 11756–11766 (2006).
He, X. S. et al. Analysis of the frequencies and of the memory T cell phenotypes of human CD8+ T cells specific for influenza A viruses. J. Infect. Dis. 187, 1075–1084 (2003).
Amyes, E. et al. Characterization of the CD4+ T cell response to Epstein–Barr virus during primary and persistent infection. J. Exp. Med. 198, 903–911 (2003).
Callan, M. F. et al. CD8+ T-cell selection, function, and death in the primary immune response in vivo. J. Clin. Invest. 106, 1251–1261 (2000).
Hillaire, M. L. et al. Characterization of the human CD8+ T cell response following infection with 2009 pandemic influenza H1N1 virus. J. Virol. 85, 12057–12061 (2011).
Miller, J. D. et al. Human effector and memory CD8+ T cell responses to smallpox and yellow fever vaccines. Immunity 28, 710–722 (2008). This study shows the generation of virus-specific effector and memory CD8+ T cell responses in the peripheral blood at sequential time points in humans following yellow fever vaccination.
Jaimes, M. C. et al. Frequencies of virus-specific CD4+ and CD8+ T lymphocytes secreting γ-interferon after acute natural rotavirus infection in children and adults. J. Virol. 76, 4741–4749 (2002).
Bont, L. et al. Natural reinfection with respiratory syncytial virus does not boost virus-specific T-cell immunity. Pediatr. Res. 52, 363–367 (2002).
de Waal, L. et al. Moderate local and systemic respiratory syncytial virus-specific T-cell responses upon mild or subclinical RSV infection. J. Med. Virol. 70, 309–318 (2003).
Gonzalez, P. A. et al. Respiratory syncytial virus impairs T cell activation by preventing synapse assembly with dendritic cells. Proc. Natl Acad. Sci. USA 105, 14999–15004 (2008).
Reed, J. R. et al. Telomere erosion in memory T cells induced by telomerase inhibition at the site of antigenic challenge in vivo. J. Exp. Med. 199, 1433–1443 (2004).
Vukmanovic-Stejic, M. et al. Varicella zoster-specific CD4+Foxp3+ T cells accumulate after cutaneous antigen challenge in humans. J. Immunol. 190, 977–986 (2013).
de Bree, G. J. et al. Characterization of CD4+ memory T cell responses directed against common respiratory pathogens in peripheral blood and lung. J. Infect. Dis. 195, 1718–1725 (2007).
de Bree, G. J. et al. Selective accumulation of differentiated CD8+ T cells specific for respiratory viruses in the human lung. J. Exp. Med. 202, 1433–1442 (2005). This report describes the initial finding of biased distribution of memory T cells that are specific for a lung pathogen in the lungs compared with in the peripheral blood.
Piet, B. et al. CD8+ T cells with an intraepithelial phenotype upregulate cytotoxic function upon influenza infection in human lung. J. Clin. Invest. (2011).
Zhu, J. et al. Virus-specific CD8+ T cells accumulate near sensory nerve endings in genital skin during subclinical HSV-2 reactivation. J. Exp. Med. 204, 595–603 (2007).
Molberg, O. et al. CD4+ T cells with specific reactivity against astrovirus isolated from normal human small intestine. Gastroenterology. 114, 115–122 (1998).
Sewell, A. K. Why must T cells be cross-reactive? Nature Rev. Immunol. 12, 669–677 (2012).
Lee, L. Y. et al. Memory T cells established by seasonal human influenza A infection cross-react with avian influenza A (H5N1) in healthy individuals. J. Clin. Invest. 118, 3478–3490 (2008).
Roti, M. et al. Healthy human subjects have CD4+ T cells directed against H5N1 influenza virus. J. Immunol. 180, 1758–1768 (2008). References 113 and 114 show that there is cross-reactivity in memory CD4+ T cells and identifies pre-existing memory T cells that are specific for avian influenza virus in individuals who never were exposed to this virus.
Su, L. F., Kidd, B. A., Han, A., Kotzin, J. J. & Davis, M. M. Virus-specific CD4+ memory-phenotype T cells are abundant in unexposed adults. Immunity 38, 373–383 (2013). This article shows cross-reactivity of virus-specific memory T cells using tetramer enrichment and identifies HIV-specific memory T cells in individuals who were never infected with this virus.
D'Orsogna, L. J., Roelen, D. L., Doxiadis, I. I. & Claas, F. H. Alloreactivity from human viral specific memory T-cells. Transpl. Immunol. 23, 149–155 (2010).
Wucherpfennig, K. W. T cell receptor crossreactivity as a general property of T cell recognition. Mol. Immunol. 40, 1009–1017 (2004).
Burrows, S. R., Khanna, R., Burrows, J. M. & Moss, D. J. An alloresponse in humans is dominated by cytotoxic T lymphocytes (CTL) cross-reactive with a single Epstein–Barr virus CTL epitope: implications for graft-versus-host disease. J. Exp. Med. 179, 1155–1161 (1994).
Wucherpfennig, K. W. & Strominger, J. L. Molecular mimicry in T cell-mediated autoimmunity: viral peptides activate human T cell clones specific for myelin basic protein. Cell 80, 695–705 (1995).
Welsh, R. M. & Selin, L. K. No one is naive: the significance of heterologous T-cell immunity. Nature Rev. Immunol. 2, 417–426 (2002).
Clute, S. C. et al. Cross-reactive influenza virus-specific CD8+ T cells contribute to lymphoproliferation in Epstein–Barr virus-associated infectious mononucleosis. J. Clin. Invest. 115, 3602–3612 (2005).
Maynard, C. L., Elson, C. O., Hatton, R. D. & Weaver, C. T. Reciprocal interactions of the intestinal microbiota and immune system. Nature 489, 231–241 (2012).
Duchmann, R. et al. T cell specificity and cross reactivity towards enterobacteria, Bacteroides, Bifidobacterium, and antigens from resident intestinal flora in humans. Gut 44, 812–818 (1999).
Hand, T. W. et al. Acute gastrointestinal infection induces long-lived microbiota-specific T cell responses. Science 337, 1553–1556 (2012).
Hammarlund, E. et al. Duration of antiviral immunity after smallpox vaccination. Nature Med. 9, 1131–1137 (2003). This study provides direct evidence that human memory T cells that are generated through vaccination are long-lived without repeat antigen exposures.
Surh, C. D. & Sprent, J. Homeostasis of naive and memory T cells. Immunity 29, 848–862 (2008).
Bushar, N. D., Corbo, E., Schmidt, M., Maltzman, J. S. & Farber, D. L. Ablation of SLP-76 signaling after T cell priming generates memory CD4 T cells impaired in steady-state and cytokine-driven homeostasis. Proc. Natl Acad. Sci. USA 107, 827–831 (2010).
Kassiotis, G., Garcia, S., Simpson, E. & Stockinger, B. Impairment of immunological memory in the absence of MHC despite survival of memory T cells. Nature Immunol. 3, 244–250 (2002).
Kassiotis, G., Gray, D., Kiafard, Z., Zwirner, J. & Stockinger, B. Functional specialization of memory TH cells revealed by expression of integrin CD49b. J. Immunol. 177, 968–975 (2006).
Macallan, D. C. et al. Measurement and modeling of human T cell kinetics. Eur. J. Immunol. 33, 2316–2326 (2003).
Macallan, D. C. et al. Rapid turnover of effector-memory CD4+ T cells in healthy humans. J. Exp. Med. 200, 255–260 (2004).
De Boer, R. J. & Perelson, A. S. Quantifying T lymphocyte turnover. J. Theor. Biol. 327, 45–87 (2013). This article contains an interesting mathematical analysis of human T cell proliferation studies.
Vukmanovic-Stejic, M. et al. Human CD4+ CD25hi Foxp3+ regulatory T cells are derived by rapid turnover of memory populations in vivo. J. Clin. Invest. 116, 2423–2433 (2006).
Weng, N. P., Levine, B. L., June, C. H. & Hodes, R. J. Human naive and memory T lymphocytes differ in telomeric length and replicative potential. Proc. Natl Acad. Sci. USA 92, 11091–11094 (1995).
Weng, N. P., Araki, Y. & Subedi, K. The molecular basis of the memory T cell response: differential gene expression and its epigenetic regulation. Nature Rev. Immunol. 12, 306–315 (2012).
Miconnet, I. Probing the T-cell receptor repertoire with deep sequencing. Curr. Opin. HIV AIDS. 7, 64–70 (2012).
Youngblood, B., Davis, C. W. & Ahmed, R. Making memories that last a lifetime: heritable functions of self-renewing memory CD8 T cells. Int. Immunol. 22, 797–803 (2010).
Robins, H. S. et al. Comprehensive assessment of T-cell receptor β-chain diversity in αβ T cells. Blood 114, 4099–4107 (2009).
Robins, H. S. et al. Overlap and effective size of the human CD8+ T cell receptor repertoire. Sci. Transl. Med. 2, 47ra64 (2010).
Siegel, A. M. et al. A critical role for STAT3 transcription factor signaling in the development and maintenance of human T cell memory. Immunity 35, 806–818 (2011).
Zinkernagel, R. M. Immunological memory not equal protective immunity. Cell. Mol. Life Sci. 69, 1635–1640 (2012).
Wilkinson, T. M. et al. Preexisting influenza-specific CD4+ T cells correlate with disease protection against influenza challenge in humans. Nature Med. 18, 274–280 (2012). The authors of this paper carried out a live challenge study using the influenza virus in human subjects and establish that reduced illness correlates with the quantity of circulating influenza virus-specific memory CD4+ T cells.
Lumsden, J. M. et al. Protective immunity induced with the RTS,S/AS vaccine is associated with IL-2 and TNF-α producing effector and central memory CD4 T cells. PLoS ONE. 6, e20775 (2011).
Hansen, S. G. et al. Cytomegalovirus vectors violate CD8+ T cell epitope recognition paradigms. Science 340, 1237874 (2013). This study shows that vaccination with CMV-based vectors expressing an HIV Gag protein generates robust effector-memory CD8+ T cell responses that have a remarkably broad specificity to epitopes presented by MHC class I and class II molecules in a non-human primate model.
Hansen, S. G. et al. Profound early control of highly pathogenic SIV by an effector memory T-cell vaccine. Nature 473, 523–527 (2011).
Hansen, S. G. et al. Immune clearance of highly pathogenic SIV infection. Nature 502, 100–104 (2013).
Sallusto, F., Lanzavecchia, A., Araki, K. & Ahmed, R. From vaccines to memory and back. Immunity 33, 451–463 (2010).
Altman, J. D. et al. Phenotypic analysis of antigen-specific T lymphocytes. Science 274, 94–96 (1996).
Bakker, A. H. & Schumacher, T. N. MHC multimer technology: current status and future prospects. Curr. Opin. Immunol. 17, 428–433 (2005).
Tan, L. C. et al. A re-evaluation of the frequency of CD8+ T cells specific for EBV in healthy virus carriers. J. Immunol. 162, 1827–1835 (1999).
Bendall, S. C. et al. Single-cell mass cytometry of differential immune and drug responses across a human hematopoietic continuum. Science 332, 687–696 (2011).
Newell, E. W. et al. Combinatorial tetramer staining and mass cytometry analysis facilitate T-cell epitope mapping and characterization. Nature Biotech. 31, 623–629 (2013).
Acknowledgements
The authors wish to thank J. Thome and D. Turner for a critical review of the manuscript. D.L.F. is supported by US National Institutes of Health grants AI106697, AI100119 and AI083022.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Glossary
- Memory homeostasis
-
The stable maintenance of memory T cell numbers through multiple mechanisms, including continuous turnover, responses to homeostatic cytokines and non-cognate T cell receptor interactions.
- Immunosenescence
-
The decreased function of the immune system with age. In particular, the number of naive T cells decreases as thymic function decreases.
- ELISPOT
-
(Enzyme-linked immunosorbent spot). An antibody capture-based method for enumerating specific CD4+ and CD8+ T cells that secrete a particular cytokine (often interferon-γ).
- MHC tetramer
-
A method of visualizing antigen-specific T cells by flow cytometry. Typically, four MHC molecules with their associated peptides are held together by streptavidin (that has four binding sites for biotin), which is attached to the tail of the MHC molecule. These four peptide—MHC complexes (tetramers) can bind to peptide-specific T cell receptors. The streptavidin molecules are often labelled with a fluorochrome so that binding can be assessed by flow cytometry.
- Telomeres
-
Regions of highly repetitive DNA at the end of linear eukaryotic chromosomes. They protect the ends of the chromosome from shortening following replication.
Rights and permissions
About this article
Cite this article
Farber, D., Yudanin, N. & Restifo, N. Human memory T cells: generation, compartmentalization and homeostasis. Nat Rev Immunol 14, 24–35 (2014). https://doi.org/10.1038/nri3567
Published:
Issue Date:
DOI: https://doi.org/10.1038/nri3567
This article is cited by
-
IL-2-free tumor-infiltrating lymphocyte therapy with PD-1 blockade demonstrates potent efficacy in advanced gynecologic cancer
BMC Medicine (2024)
-
Exosomal miRNA-mediated intercellular communications and immunomodulatory effects in tumor microenvironments
Journal of Biomedical Science (2023)
-
TET2 guards against unchecked BATF3-induced CAR T cell expansion
Nature (2023)
-
Regulation of T cells by myeloid-derived suppressor cells: emerging immunosuppressor in lung cancer
Discover Oncology (2023)
-
The role of the adaptive immune system and T cell dysfunction in neurodegenerative diseases
Journal of Neuroinflammation (2022)