Abstract
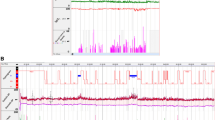
We investigated blood pressure (BP) variability as assessed by beat-to-beat, reading-to-reading and day-to-day BP variability indices in patients with obstructive sleep apnea-hypopnea syndrome (OSAHS). In 786 hospitalized hypertensives (mean age, 53.2 years; 42.2% women), we performed 10-min beat-to-beat (n = 705), 24-h ambulatory (n = 779), and 7-day home BP (n = 445) measurements and the full overnight polysomnography. Mild, moderate and severe OSAHS were defined as an apnea-hypopnea index of 5–14, 15–29, and ≥ 30 events per hour, respectively. BP variability indices including variability independent of the mean (VIM), average real variability (ARV), and maximum–minimum difference (MMD), were compared across the OSAHS severity groups. In univariate analysis, beat-to-beat systolic VIM and MMD, reading-to-reading asleep systolic and diastolic ARV and MMD increased from patients without OSAHS, to patients with mild, moderate and severe OSAHS. This increasing trend for beat-to-beat systolic VIM and MMD remained statistically significant after adjustment for confounders (P ≤ 0.047). There was significant (P ≤ 0.039) interaction of the presence and severity of OSAHS with age and body mass index in relation to the beat-to-beat systolic VIM and MMD and with the presence of diabetes mellitus in relation to asleep systolic ARV. The association was stronger in younger (age < 50 years) and obese (body mass index ≥ 28 kg/m²) and diabetic patients. None of the day-to-day BP variability indices reached statistical significance (P ≥ 0.16). BP variability, in terms of beat-to-beat systolic VIM and MMD and asleep reading-to-reading asleep systolic ARV, were higher with the more severe OSAHS, especially in younger and obese and diabetic patients.

This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Peppard PE, Young T, Palta M, Skatrud J. Prospective study of the association between sleep-disordered breathing and hypertension. N Engl J Med. 2000;342:1378–84.
Cowie MR, Linz D, Redline S, Somers VK, Simonds AK. Sleep disordered breathing and cardiovascular disease: JACC state-of-the-art review. J Am Coll Cardiol. 2021;78:608–24.
Chen Q, Cheng YB, Liu CY, Guo QH, Xu SK, Huang QF, et al. Ambulatory blood pressure in relation to oxygen desaturation index as simultaneously assessed by nighttime finger pulse oximetry at home. J Clin Hypertens. 2018;20:648–55.
Smith RP, Veale D, Pépin JL, Lévy PA. Obstructive sleep apnoea and the autonomic nervous system. Sleep Med Rev. 1998;2:69–92.
Misaka T, Niimura Y, Yoshihisa A, Wada K, Kimishima Y, Yokokawa T, et al. Clinical impact of sleep-disordered breathing on very short-term blood pressure variability determined by pulse transit time. J Hypertens. 2020;38:1703–11.
Pal A, Martinez F, Aguila AP, Akey MA, Chatterjee R, Conserman MGE, et al. Beat-to-beat blood pressure variability in patients with obstructive sleep apnea. J Clin Sleep Med. 2021;17:381–92.
Steinhorst AP, Gonçalves SC, Oliveira AT, Massierer D, Gus M, Fuchs SC, et al. Influence of sleep apnea severity on blood pressure variability of patients with hypertension. Sleep Breath. 2014;18:397–401.
Martynowicz H, Porębska I, Poręba R, Mazur G, Brzecka A. Nocturnal blood pressure variability in patients with obstructive sleep apnea syndrome. Adv Exp Med Biol. 2016;952:9–15.
Shao L, Heizhati M, Yao X, Wang Y, Abulikemu S, Zhang D, et al. Influences of obstructive sleep apnea on blood pressure variability might not be limited only nocturnally in middle-aged hypertensive males. Sleep Breath. 2018;22:377–84.
Shiina K, Tomiyama H, Takata Y, Matsumoto C, Odaira M, Kato K, et al. Obstructive sleep apnea as possible causal factor for visit-to-visit blood pressure variability. Circ J. 2016;80:1787–94.
Kansui Y, Matsumura K, Morinaga Y, Inoue M, Sakata S, Oishi E, et al. Impact of obstructive sleep apnea on long-term blood pressure variability in Japanese men: a cross-sectional study of a work-site population. Hypertens Res. 2018;41:957–64.
Wei FF, Li Y, Zhang L, Xu TY, Ding FH, Wang JG, et al. Beat-to-beat, reading-to-reading, and day-to-day blood pressure variability in relation to organ damage in untreated Chinese. Hypertension. 2014;63:790–6.
Stevens SL, Wood S, Koshiaris C, Law K, Glasziou P, Stevens RJ, et al. Blood pressure variability and cardiovascular disease: systematic review and meta-analysis. BMJ. 2016;354:i4098.
Webb AJS, Mazzucco S, Li L, Rothwell PM. Prognostic significance of blood pressure variability on beat-to-beat monitoring after transient ischemic attack and stroke. Stroke. 2018;49:62–7.
World Medical A. World Medical Association Declaration of Helsinki: ethical principles for medical research involving human subjects. JAMA. 2013;310:2191–4.
Xu L, Han F, Keenan BT, Kneeland-Szanto E, Yan H, Dong X, et al. Validation of the Nox-T3 portable monitor for diagnosis of obstructive sleep apnea in Chinese adults. J Clin Sleep Med. 2017;13:675–83.
Kapur VK, Auckley DH, Chowdhuri S, Kuhlmann DC, Mehra R, Ramar K, et al. Clinical practice guideline for diagnostic testing for adult obstructive sleep apnea: An American Academy of sleep medicine clinical practice guideline. J Clin Sleep Med. 2017;13:479–504.
Rothwell PM, Howard SC, Dolan E, O’Brien E, Dobson JE, Dahlöf B, et al. Prognostic significance of visit-to-visit variability, maximum systolic blood pressure, and episodic hypertension. Lancet. 2010;375:895–905.
Mena L, Pintos S, Queipo NV, Aizpúrua JA, Maestre G, Sulbarán T. A reliable index for the prognostic significance of blood pressure variability. J Hypertens. 2005;23:505–11.
ElSayed NA, Aleppo G, Aroda VR, Bannuru RR, Brown FM, Bruemmer D, et al. 2. Classification and diagnosis of diabetes: standards of care in diabetes-2023. Diabetes Care. 2023;46:S19–40.
Misaka T, Yoshihisa A, Yokokawa T, Takeishi Y. Effects of continuous positive airway pressure on very short-term blood pressure variability associated with sleep-disordered breathing by pulse transit time-based blood pressure measurements. J Hypertens. 2023;41:733–40.
Bonsignore MR, Parati G, Insalaco G, Castiglioni P, Marrone O, Romano S, et al. Baroreflex control of heart rate during sleep in severe obstructive sleep apnoea: effects of acute CPAP. Eur Respir J. 2006;27:128–35.
Bonsignore MR, Parati G, Insalaco G, Marrone O, Castiglioni P, Romano S, et al. Continuous positive airway pressure treatment improves baroreflex control of heart rate during sleep in severe obstructive sleep apnea syndrome. Am J Respir Crit Care Med. 2002;166:279–86.
Parati G, Stergiou GS, Dolan E, Bilo G. Blood pressure variability: clinical relevance and application. J Clin Hypertens 2018;20:1133–7.
Dissanayake HU, Bin YS, Ucak S, de Chazal P, Sutherland K, Cistulli PA. Association between autonomic function and obstructive sleep apnea: a systematic review. Sleep Med Rev. 2021;57:101470.
Kajikawa M, Higashi Y. Obesity and endothelial function. Biomedicines. 2022;10:1745.
Pugliese G, Barrea L, Laudisio D, Salzano C, Aprano S, Colao A, et al. Sleep apnea, obesity, and disturbed glucose homeostasis: Epidemiologic evidence, biologic insights, and therapeutic strategies. Curr Obes Rep. 2020;9:30–38.
Neahring JM, Stepniakowski K, Greene AS, Egan BM. Insulin does not reduce forearm alpha-vasoreactivity in obese hypertensive or lean normotensive men. Hypertension. 1993;22:584–90.
Myers MG, Stergiou GS. Reporting bias: Achilles’ heel of home blood pressure monitoring. J Am Soc Hypertens. 2014;8:350–7.
Mena LJ, Felix VG, Melgarejo JD, Maestre GE. 24-hour blood pressure variability assessed by average real variability: a systematic review and meta-analysis. J Am Heart Assoc. 2017;6:e006895.
Acknowledgements
The authors gratefully acknowledge the voluntary participation of all study participants and the expert technical assistance of Yu-Ting Jiang, Bang-Qing Xiao, Jun-Wei Li, Bei-Wen Lv (Shanghai Institute of Hypertension, Shanghai, China).
Funding
The study investigators were financially supported by grants from the National Natural Science Foundation of China (82070432, 82070435, 82270469, and 82370426), and Ministry of Science and Technology (2018YFC1704902 and 2022YFC3601302), Beijing, China, from the Shanghai Commissions of Science and Technology (grant 19DZ2340200, 22S31905100), and Health (grant 20234Y0036, “Three-year Action Program of Shanghai Municipality for Strengthening the Construction of Public Health System” GWV-10.1-XK05 and a special grant for “leading academics”), Shanghai, China, and from the Clinical Research Program, Ruijin Hospital, Shanghai Jiao Tong University School of Medicine (grant 2018CR010), Shanghai, China.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Cheng, YB., Guo, QH., Xia, JH. et al. Obstructive sleep apnea in relation to beat-to-beat, reading-to-reading, and day-to-day blood pressure variability. Hypertens Res 47, 1391–1400 (2024). https://doi.org/10.1038/s41440-024-01628-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41440-024-01628-4
Keywords
This article is cited by
-
Hypertension and blood pressure variability in patients with obstructive sleep apnea
Hypertension Research (2024)