Impact
-
This article summarizes the adverse effects of climate and environmental change on children’s health.
-
We call for policy change, education, and advocacy to halt further deterioration of planetary health and for specific measures to prevent the negative effects of climate and environmental change on children’s health.
-
We offer an agenda for research, policy change, and healthcare practices to improve the resilience of pediatric populations in the face of climate change.
Similar content being viewed by others
Since the beginning of the industrial age, humans have accelerated the release of greenhouse gases such as carbon dioxide, methane, nitrous oxides, and fluorinated gases through the increased burning of fossil fuels. Between 1900 and 2000, fossil fuel usage increased 16 fold; between 2000 and 2019, it further increased 1.5 fold.1 In 2020, the annual rate of increase of CO2 emissions was about 100 times faster than previous natural increases, which occurred at the end of the last ice age.2 The Intergovernmental Panel On Climate Change concluded that anthropogenic (caused by human activity) greenhouse gas emissions were responsible for approximately 1.1 °C of warming since 1850–1900.3 By 2100, global temperature increases between 1.4 and 4.4 °C above preindustrial temperatures are predicted under the best and worst greenhouse gas emission scenarios, respectively.3
With increasing global temperatures, the severity and frequency of wildfires, flooding, sea level rise, heatwaves and hurricanes have increased and are expected to worsen further. In Australia, between 1950 and 2016, heatwaves became more intense with increases in peak temperature, and more frequent and longer events.4 Glaciers have been melting at a rapid pace and it is estimated that glacier mass loss was at least 10 times more likely to have occurred in 2018 due to anthropogenic influence than without.5 In the United States, two million hectares of forest and other ecosystems burnt annually between 1992 and 2001; between 2002 and 2011, this increased to three million hectares.6 Using the Berkeley Earth temperature dataset and key heatwave metrics, measures of cumulative heat show significant increases almost everywhere since the 1950s, mainly driven by heatwave days.7 Record temperatures in 2020 resulted in 626 million more person-days affecting children younger than 1 year, compared with the annual average for the 1986–2005 baseline.8
While fossil fuels are major contributors to climate change, other human activities such as deforestation, urbanization, and the release of chemicals and effluents from mining, agriculture, and manufacturing are also having significant effects on the environment. Forests are natural carbon sinks, and their destruction reduces the earth’s ability to absorb the excess carbon generated. Oceans also act as carbon sinks, absorbing excess CO2. The ocean’s average pH has decreased by 0.1 units, which represents a 30% increase in acidity since preindustrial times.9 The increased acidity is particularly detrimental to marine invertebrate species such as coral, sea urchins and other species requiring carbonate to build their shells. Ocean acidification and loss of these organisms threaten to disrupt marine ecosystems.
Climate change and human health
Human health is adversely affected by climate change. Exposure to heatwaves can cause cerebral edema, exercise-induced muscle cramps, rash, rhabdomyolysis, syncope, and life-threatening stroke. In Hyderabad, India, a city of around 10 million, analysis of data between 2006 and 2015 found that the mean number of deaths per day was 16% (14.6 mean deaths per day) higher when the maximum daily temperature was >40 °C compared to <35 °C.10 Wildfires increase levels of fine particulate matter (2.5 μm and smaller) and other toxic chemicals from structures that burn.11 These fine particles are small enough to enter the lungs and bloodstream, increasing risk of respiratory and cardiovascular diseases. Epidemiological studies show that increased exposure to fine particulate matter increases risks of chronic and acute adverse health outcomes.12 Climate change has altered the geographical distribution of pollen and increased pollen season duration and allergenicity, increasing allergic disorders.13 Thunderstorms increase allergenicity of pollen leading to the phenomenon of thunderstorm asthma. Thunderstorms and lightning during the aeroallergen season cause pollen to rupture increasing concentrations of smaller respirable allergenic particles that cause acute asthma exacerbations.14 Drought adversely affects human health as food and water shortages increase risk of malnutrition and dehydration. Increases in the geographic range of infectious vectors from tropical to subtropical and temperate climates alter the risk of vector-borne diseases such as Zika and Dengue.15 These environmental changes will exacerbate political and social instability, climate migration, and disputes over scarce resources increasing health risks and access to healthcare.16 Climate change is a “threat multiplier” that forces vulnerable populations who have the least resources to adapt or risk displacement. The most displaced populations are likely to end up in cities, contributing to rapid urbanization and expansion into informal settlements, bereft of governmental services.17
Environmental pollutants and human health
Increased levels of anthropogenic pollutants are also having adverse effects on human health. We are increasingly exposed to expanding array of toxic pollutants. In 2020, 230 million tons of chemicals produced in the European Union were classified as hazardous to health.18 Many of these are novel chemicals that the human body has never encountered before. These chemicals now contaminate the air we breathe, the water we drink, and the soil that feeds the plants that produce the foods we eat. The World Health Organization estimates that over 93% of the world’s children under the age of 15 breathe air so polluted that it puts their health and development at serious risk.19 Microplastics and nanoplastics, defined as those <5 mm and <0.1 µm, respectively, are of major environmental concern because of their ubiquitous presence. As of 2015, estimates indicate that about 6300 million metric tons of plastic waste were generated, the majority of which end up polluting the environment. Nanoplastics enter tissues due to their small size; they have been detected in human lung, placenta, and blood tissue and are potentially harmful to human health.20 Furthermore, plastics persist in the environment because they are resistant to environmental degradation, leading to accumulation over time. Also, many of the additives used to manufacture plastics for improving strength and functionality are toxic and these eventually leech into the environment as well.
Increased vulnerability of children to the effects of climate change and environmental pollutants
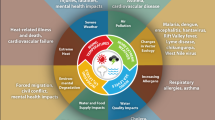
Infants and children are particularly vulnerable to the effects of pollution and climate change, due to their increased metabolic rate, rapid rate of growth and development, undeveloped detoxification mechanisms, immature immune system, and increased exposure to toxins due to time spent outdoors. Children from socio-economically disadvantaged backgrounds are at greater risk because they are less likely to have access to clean water and nutritious food, and more likely to live under unhygienic conditions. The urban poor are also likely to live near highly polluted industrial areas or near high-traffic areas. Figure 1 depicts the effects of climate change and environmental pollutants on maternal and child health outcomes. Poor health during infancy and childhood has long-lasting adverse consequences that affect aspects of their future, and can result in a lifetime of lost opportunities.21
The 2021 UNICEF “Children’s Climate Risk Index” estimates that globally, 9 in 10 children are exposed to air pollution at levels that exceeds 10 μg/m3; 1 in 3 are exposed to heatwaves, water scarcity, and lead poisoning; 1 in 4 are exposed to vector-borne diseases; 1 in 6 are affected by cyclones; 1 in 7 are exposed to riverine flooding; and 1 in 10 are exposed to coastal flooding.22 The majority (88%) of the global burden of climate-sensitive health outcomes occurs in children under 5 years of age.23 The risk to the child starts during fetal development; maternal exposure to fine particulate air pollution or high environmental temperature increases the risk of preterm birth and low birth weight.24,25 Air pollutant exposure at levels commonly experienced in European populations is associated with placental gene methylation and increased risk of preeclampsia.26
Future climate projections and the need for global efforts to combat climate change and environmental degradation
The 2015 Paris Agreement under the United Nations Framework Convention on Climate Change was a major milestone, with countries agreeing to pursue actions to limit global temperature increase to well below 2.0 °C above preindustrial temperatures, and to aim to limit the increase to 1.5 °C in 2100. However, 7 years later, many challenges to meeting these goals remain. Current promises and actions by countries to limit climate change are insufficient to meet the goals of the Paris Agreement.27
There is an urgent need to act at all levels from international communities to industry to professional organizations to individuals. The pediatrics-based healthcare system is trying to respond to climate change28 by certain adaptation techniques and caregivers are trying to respond to casualties in climate change events. However, the healthcare industry needs to identify the industry’s major sources of greenhouse gas emissions and pollutants. We need a call to action for healthcare providers to reevaluate processes and systems to deliver the best possible health outcomes while doing no harm to the planet. Increased research, education, policy, and advocacy are needed.
In an effort to educate and focus on research needs in climate change and children’s health, Pediatric Research is publishing a series of articles on climate change and environmental pollutants selected by the editors and authors of this scoping paper. Future directions for research, policy, and healthcare practices to improve the resilience of the pediatric population in the face of climate change are listed in Box 1.
References
Our world in data. Global Fossil Fuel Consumption https://ourworldindata.org/fossil-fuels (2022).
Climate.gov. Climate Change: Atmospheric Carbon Dioxide https://www.climate.gov/news-features/understanding-climate/climate-change-atmospheric-carbon-dioxide (2022).
IPCC. Climate Change Widespread, Rapid, and Intensifying – IPCC https://www.ipcc.ch/2021/08/09/ar6-wg1-20210809-pr/ (2021).
Trancoso, R. et al. Heatwaves intensification in Australia: a consistent trajectory across past, present and future. Sci. Total Environ. 742, 140521 (2020).
Vargo, L. J. et al. Anthropogenic warming forces extreme annual glacier mass loss. Nat. Clim. Change 10, 856–861 (2020).
Liu, Y., Goodrick, S. L. & Stanturf, J. A. Future U.S. wildfire potential trends projected using a dynamically downscaled climate change scenario. For. Ecol. Manag. 294, 120–135 (2013).
Perkins-Kirkpatrick, S. E. & Lewis, S. C. Increasing trends in regional heatwaves. Nat. Commun. 11, 3357 (2020).
Romanello, M. et al. The 2021 report of the Lancet countdown on health and climate change: code red for a healthy future. Lancet 398, 1619–1662 (2021).
National Oceanic and Atmospheric Administration. Ocean Acidification https://www.noaa.gov/education/resource-collections/ocean-coasts/ocean-acidification (2020).
Mazdiyasni, O. et al. Increasing probability of mortality during indian heat waves. Sci. Adv. 3, e1700066 (2017).
EPA. Estimate of Pollutant Emissions from Fires in the Wildland Urban Interface https://cfpub.epa.gov/si/si_public_record_report.cfm?dirEntryId=349539&Lab=CEMM (2020).
Mukherjee, A. & Agrawal, M. A global perspective of fine particulate matter pollution and its health effects. Rev. Environ. Contam Toxicol. 244, 5–51 (2018).
D’Amato, G. et al. The effects of climate change on respiratory allergy and asthma induced by pollen and mold allergens. Allergy 75, 2219–2228 (2020).
Harun, N. S., Lachapelle, P. & Douglass, J. Thunderstorm-triggered asthma: what we know so far. J. Asthma Allergy 12, 101–108 (2019).
Semenza, J. C. & Suk, J. E. Vector-borne diseases and climate change: a European perspective. FEMS Microbiol. Lett. 365, fnx244 (2018).
Agache, I. et al. Climate change and global health: a call to more research and more action. Allergy 77, 1389–1407 (2022).
UNHCR, The UN Refugee Agency. Global Trends: Forced Displacement in 2018 https://www.unhcr.org/globaltrends2018/ (2018).
Eurostat. Statistics Explained. Chemicals Production and Consumption Statistics https://ec.europa.eu/eurostat/statistics-explained/index.php?title=Chemicals_production_and_consumption_statistics#Total_production_of_chemicals (2021).
World Health Organization. More Than 90% of the World’s Children Breathe Toxic Air Every Day https://www.who.int/news/item/29-10-2018-more-than-90-of-the-worlds-children-breathe-toxic-air-every-day (2018).
Wright, S. L. & Kelly, F. J. Plastic and human health: a micro issue? Environ. Sci. Technol. 51, 6634–6647 (2017).
Perera, F. & Nadeau, K. Climate change, fossil-fuel pollution, and children’s health. N. Engl. J. Med. 386, 2303–2314 (2022).
UNICEF. The Climate Crisis Is a Child Rights Crisis https://www.unicef.org/media/105376/file/UNICEF-climate-crisis-child-rights-crisis.pdf (2021).
Sheffield, P. E. & Landrigan, P. J. Global climate change and children’s health: threats and strategies for prevention. Environ. Health Perspect. 119, 291–298 (2011).
Li, X. et al. Association between ambient fine particulate matter and preterm birth or term low birth weight: an updated systematic review and meta-analysis. Environ. Pollut. 227, 596–605 (2017).
Ozonoff, A. et al. Phenotypes of disease severity in a cohort of hospitalized COVID-19 patients: results from the IMPACC study. eBioMedicine 83, 104208 (2022).
Abraham, E. et al. Pregnancy exposure to atmospheric pollution and meteorological conditions and placental DNA methylation. Environ. Int. 118, 334–347 (2018).
Liu, P. R. & Raftery, A. E. Country-based rate of emissions reductions should increase by 80% beyond nationally determined contributions to meet the 2 °C target. Commun. Earth Environ. 2, 29 (2021).
World Health Organization. Cop26 Special Report on Climate Change and Health: The Health Argument for Climate Action https://www.who.int/publications/i/item/9789240036727 (2021).
Funding
Financial support was provided by the Sean N. Parker Center for Allergy and Asthma Research at Stanford University, NHLBI grant P01HL152953, and NIEHS grant R01ES032253.
Author information
Authors and Affiliations
Contributions
All authors contributed to the writing and review of the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Sampath, V., Nadeau, K.C., Ebi, K.L. et al. Improving planetary health is integral to improving children’s health—a call to action. Pediatr Res (2022). https://doi.org/10.1038/s41390-022-02432-x
Received:
Revised:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41390-022-02432-x