Abstract
Hypertensive disorders of pregnancy (HDP) are common complications associated with maternal and neonatal morbidity and mortality worldwide. Insights gained from long-term cohort studies have revealed that women with a history of HDP are predisposed to recurrent HDP in subsequent pregnancies and face heightened risks for cardiovascular and metabolic diseases later in life. Pregnancy is a unique condition that overloads maternal cardiac and metabolic functions, and is recognized as a “maternal stress test” for future cardiovascular and metabolic diseases. Pregnancy and postpartum period provide a valuable opportunity for identifying women with underlying and unrecognized cardiovascular and metabolic risk factors. Establishing an effective postpartum healthcare program for women who have experienced HDP is crucial in reducing the future risk of health complications. Postpartum care consists of supportive care for both mothers and children, including not only the assessment of physical and psychological well-being but also long-term postpartum preventive health management. Interpregnancy care is a continuum from postpartum care and includes supportive care to prepare for future pregnancies. Various initiatives across nations have been initiated to establish follow-up programs for women with a history of HDP; however, sufficient evidence of the impact of such programs is not available. Substantial challenges persist in establishing an efficient postpartum follow-up program, including educational strategies, selection of effective lifestyle interventions, and collaboration among various healthcare providers. This review outlines the postpartum and interpregnancy care of women who have experienced HDP as well as the current status and challenges of related healthcare initiatives in Japan.

Similar content being viewed by others
Introduction
Hypertensive disorders of pregnancy (HDP) are one of the most common pregnancy complications associated with maternal and neonatal morbidity and mortality worldwide and are classified into four subtypes (gestational hypertension, preeclampsia, chronic hypertension, and superimposed preeclampsia) [1,2,3]. Preeclampsia, a severe type of HDP, is a multisystem progressive syndrome that manifests as hypertension, proteinuria, and various maternal end-organ dysfunctions. The main pathophysiology of preeclampsia is uteroplacental insufficiency in the early stage of pregnancy and systemic endothelial dysfunction in the second and third stages of pregnancy [4].
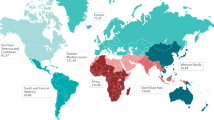
HDP account for approximately 20% of preterm births and 14.0% of maternal deaths worldwide [5, 6]. Due to the rise in advanced maternal age, pregnancy via assisted reproductive technology, obesity, and chronic hypertension, there has been a recent escalation in the prevalence of HDP [7]. According to the Centers for Disease Control and Prevention (CDC), HDP affect one in seven hospital deliveries in the United States [8].
The clinical manifestations of HDP typically resolve soon after delivery, with recovery to a non-pregnant state by 12 weeks postpartum. Nevertheless, HDP are not merely a transient health problem; approximately 20% of women who have experienced HDP present hypertension requiring antihypertensive medications for weeks to months postpartum [9,10,11]. Additionally, accumulating evidence based on long-term cohort studies over the last decade demonstrates that women who experience HDP exhibit an increased risk of recurrent HDP in subsequent pregnancies and future various cardiovascular and metabolic diseases (e.g., hypertension, heart failure, stroke, chronic kidney disease (CKD), diabetes mellitus, and hyperlipidemia), while this risk persists for a prolonged period after delivery [9, 12]. Although the need for long-term postpartum follow-up has gradually gained recognition, a comprehensive postpartum follow-up framework to mitigate the risk of recurrent HDP and future health complications in women with a history of HDP has not been fully established, although various initiatives have been undertaken in several countries [13,14,15,16,17].
International and national health organizations, including the World Health Organization and CDC, play pivotal roles in promoting preconception care as an essential component of maternal and child health [18]. In Japan, based on the provisions of the Basic Law for Child and Maternal Health and Child Development enacted in 2018, the Cabinet approved the Basic Policy on Child and Maternal Health and Child Development in 2021. The importance of the concept of preconception care has gained recognition, and initiatives toward the development of a preconception care system have gradually begun in Japan. Within this framework, attention has been directed towards interpregnancy care, also known as interconception care, which encompasses the continuum of postpartum care (Fig. 1). Postpartum care consists of supportive care for both mothers and children to promote better health and well-being and includes assessment of physical and psychological well-being, infant care and feeding, sexuality, and reproductive life planning, but also long-term postpartum preventive health management. Postpartum and well-women care share the common aim of advancing women’s health and well-being. Interpregnancy care is a continuum from postpartum care and includes supportive care to prepare for future pregnancies (Fig. 1) [13, 19].
This review presents the short- and long-term outcomes of women who have experienced HDP, discusses interpregnancy care as a strategy for preventing recurrent HDP in subsequent pregnancies, and explores postpartum care with the goal of mitigating long-lasting cardiovascular risk. Additionally, this review summarizes the current status and challenges of related postpartum and interpregnancy healthcare initiatives in Japan to improve future pregnancy outcomes and women’s health.
Definitions of postpartum and interpregnancy care
The postpartum period, usually 6–8 weeks, is associated with specific health vulnerabilities (e.g., postpartum depression, anemia, sleep deprivation, and fatigue), as postpartum women undergo substantial and rapid adaptations to a non-pregnant state [20]. Postpartum care and support through postpartum visits include not only managing the physical and psychological well-being of women and infants during the early postpartum period, but also building a foundation for their long-term health along the life course. The American College of Obstetrics and Gynecology (ACOG) recommends an initial assessment within the first three weeks postpartum, which later is followed up with ongoing care as needed, concluding with a comprehensive visit no later than 12 weeks postpartum [19]. The ACOG also emphasizes that postpartum care should provide services and support tailored to individual patient needs. Interpregnancy care can be considered as preconception care for subsequent pregnancies. Moreover, interpregnancy care is encompassed within the continuum of postpartum care provided to postpartum women who intend to have future pregnancies aiming to improve the maternal and neonatal outcomes (Fig. 1) [13]. Thus, the postpartum period presents a valuable opportunity for healthcare providers to engage in comprehensive education and guidance. Providing women with knowledge of infant care, breastfeeding, contraception, future disease risks, and recommended lifestyle adjustments can profoundly and positively impact the long-term health of both mothers and children [15, 19].
Postpartum management and short-term prognosis of HDP
Currently, the only definitive treatment for HDP remains termination of pregnancy via delivery. However, the risk of complications associated with HDP does not dissipate rapidly postpartum. In a multicenter study conducted by our group, 50.2% of women who had experienced HDP exhibited hypertension within one month postpartum, 28.5% of whom experienced severe hypertension, thereby suggesting the necessity of appropriate antihypertensive treatment not only during pregnancy but also after delivery [21].
The target blood pressure value for postpartum hypertension differs between guidelines (Japan Society for the Study of Hypertension in Pregnancy [JSSHP]: <140/90 mmHg, International Society for the Study of Hypertension in Pregnancy [ISSHP]: diastolic blood pressure ≤ 85 mmHg, ACOG: < 150/100 mmHg, National Institute for Health and Care Excellence: ≤ 135/85 mmHg) [2, 3, 22, 23]. While concerns regarding impaired placental blood flow due to excessive antihypertensive treatment during pregnancy have been raised, a proactive approach to achieve adequate blood pressure control is recommended during the postpartum period to prevent adverse maternal outcomes such as eclampsia and cerebral hemorrhage [24]. The risks of eclampsia, HELLP syndrome (hemolysis, elevated liver enzymes, and low platelet count), pulmonary edema, peripartum cardiomyopathy, and maternal death persist during the postpartum period as observed during pregnancy, underscoring the significance of comprehensive systemic management of postpartum women [25].
In terms of short-term prognosis, approximately 10–30% of all maternal deaths are attributed to HDP-related complications [8, 26, 27]. According to the nationwide registration system for maternal deaths in Japan, between 2010 and 2015, HDP accounted for 10.8% (30/277) of maternal deaths [27]. Based on data from the CDC’s National Pregnancy Mortality Surveillance System for 2011–2015 regarding the timing of HDP-related maternal deaths within one year, indicated that 10.8% of these deaths occurred during pregnancy, 19.3% on the day of delivery, 44.3% within 1–6 days postpartum, 20.8% within 7–42 days postpartum, and 4.7% at 43–365 days postpartum [26]. These results imply that nearly two-thirds of maternal deaths related to HDP occur on the day of delivery or within the first week following delivery, highlighting a greater incidence during the postpartum period compared to that observed during pregnancy. Additionally, approximately one-third of eclampsia and HELLP syndrome cases occur during the postpartum period, with HELLP syndrome being particularly common within the first 48 hours after delivery, therefore, reemphasizing the importance of postpartum maternal management [28].
Although differences exist among patients of different racial groups, blood pressure returns to pre-pregnancy levels within 6–8 weeks postpartum in most cases, rendering antihypertensive agents unnecessary. However, if hypertension or proteinuria persists beyond 12 weeks postpartum, suggesting secondary hypertension or unrecognized renal disease. Consultation with internal medicine specialists, such as cardiologists, nephrologists, or endocrinologists, for the thorough assessment and management of patients is warranted. With regards to proteinuria, the diagnostic criteria during pregnancy and postpartum (≥0.3 g/gCr) are different from that in non-pregnant women (≥0.15 g/gCr). According to the CKD practice guidelines 2018 [29], proteinuria is defined as 0.15 g/gCr or more, and patients with proteinuria are at high risk for subsequent CKD, thereby, followed up is needed. However, postpartum follow-up is generally terminated if the protein level is less than 0.3 g/gCr at postpartum checkup, therefore, women at risk for developing CKD (protein level 0.15–0.30 g/gCr) may be missed. To avoid underdiagnosing women at high risk of future CKD, the diagnostic criteria for postpartum proteinuria may require a reexamination. The JSSHP currently considers postpartum proteinuria an important issue and has initiated research on trends in proteinuria up to 12 weeks postpartum in women with preeclampsia as an academic award project.
HDP and future disease risks
Numerous long-term cohort studies have shown that women with HDP have elevated risk of cerebrovascular and cardiovascular disease (CVD), CKD, diabetes mellitus, dyslipidemia, and cognitive impairment [9, 12, 14]. According to a meta-analysis of 22 studies, women who developed preeclampsia exhibited elevated risk of future heart failure (risk ratio 4.19, 95% confidence interval [CI] [2.09–8.38]), coronary artery disease (2.50 [1.43–4.37]), cardiovascular-related mortality (2.21 [1.83–2.66]), and stroke (1.81 [1.29–2.55]) [30]. Moreover, women with a history of preeclampsia had a higher risk of type 2 diabetes mellitus (adjusted OR 2.28, 95% CI [1.58–3.28]), metabolic syndrome (4.05, [2.42–6.77]), and dyslipidemia (2.54 [0.81–2.95]) [31]. Mito et al. demonstrated that women who had experienced HDP presented a higher risk of developing hypertension five years after the index pregnancy (adjusted OR 7.1, 95% CI [2.0–25.6]) [32]. A report from Japan, using data from Maternal and Child Health Handbooks, substantiated an increased risk of CKD among women with a history of HDP [33].
Furthermore, these risks increase in women with earlier gestational week at delivery and are further accentuated in women who are accompanied by fetal growth restriction and those who have experienced HDP in two or more pregnancies [34, 35]. Moreover, CVD risk differs between different types of HDP [36]. Notably, according to a 20-year cohort study encompassing 1.3 million women in the United Kingdom (the CALIBER study), 65% of the first cerebrovascular and cardiovascular events occurred in women under 40 years of age with a history of preeclampsia [37]. Furthermore, this risk was evident as early as one year after the index pregnancy, underscoring the necessity for early postpartum surveillance and intervention for risk reduction. Regarding cognitive impairments, HDP is associated with poor working memory, verbal learning, and cognitive disorders, particularly of vascular cognitive impairment [38, 39]. However, the caveat is that several reports indicate that the magnitude of these increased risks is significantly reduced when appropriately adjusting for the presence of postpartum hypertension or pre-pregnancy potential confounding factors that are related to such disorders [40, 41]. This implies that a certain proportion of the influence of HDP on future risk is potentially mediated by subsequent hypertension and pre-pregnancy factors.
The blood pressure levels of women with HDP essentially return to normal within the initial 12 weeks postpartum, often leading both patients and clinicians to discontinue surveillance. Therefore, adequate follow-up even after blood pressure level returns to the normal range is warranted for women with a history of HDP.
Nevertheless, the Japanese Society of Hypertension recommends inquiring about the history of pregnancy complications, including HDP, gestational diabetes mellitus, and proteinuria, when obtaining medical history from women with hypertension [42]. Similarly, the American College of Cardiology/American Heart Association (ACC/AHA) guidelines stipulate that a history of preeclampsia is a key factor contributing to an elevated risk of CVD [43].
Mechanisms underlying elevated future cardiovascular risk in women with a history of HDP
Risk factors for HDP include advanced maternal age, obesity, diabetes mellitus, kidney diseases, autoimmune diseases, and familial history of hypertension [1, 4]. These risk factors are shared with those of CVD and metabolic diseases, suggesting that the inherent predispositions of individuals play a significant role in the development of HDP, future CVD, and metabolic syndrome [44]. It has been hypothesized that women harboring inherent predisposition for these diseases are susceptible to manifest HDP due to pregnancy-related physiological changes such as increased cardiac volume overload, insulin resistance, inflammatory cytokines, oxidative stress, and activated renin-angiotensin-aldosterone system (Fig. 2) [45]. The maternal inability (i.e., the development of HDP) to adapt to these dramatic physiological changes can uncover underlying and often unrecognized CVD or metabolic disease risks [46]. Therefore, pregnancy imposes a stress burden on maternal physiology, with the ensuing pregnancy complications acting as harbors of future CVD. Consequently, pregnancy is often regarded as a “maternal stress test.”
However, there are several reports suggesting that the onset of HDP itself triggers the progression of systemic endothelial dysfunction, myocardial impairment, and hepatic and renal dysfunction during pregnancy, consequently heightening the risk of subsequent CVD (Fig. 2) [47]. This is exemplified by cases in which some women who experience HDP exhibit prolonged hypertension and proteinuria postpartum, or in which some women with CKD experience exacerbated renal function during pregnancy and for a long time after delivery. Such cases imply that pregnancy itself or the manifestation of HDP potentially imparts a long-lasting burden on cardiac and renal functions.
Our preclinical research, employing a rat model of preeclampsia, revealed that preeclampsia induces postpartum left ventricular hypertrophy, elevated markers of cardiac hypertrophy, and alterations in the proteome linked to lipid abnormalities, hypertension, and arterial sclerosis, underscoring that the development of preeclampsia, regardless of pre-pregnancy potential predisposition, is associated with an elevated risk of future CVD [48, 49]. These studies revealed that “aberrant inflammation” during pregnancy, one of the key mechanisms underlying the onset of preeclampsia, contributes to an increased risk of future CVD.
In summary, the mechanisms contributing to the heightened risk of CVD in women with a history of HDP involve two main aspects: (1) women who have experienced HDP have a variety of potential risk factors for CVD before pregnancy, and (2) end-organ dysfunction and long-lasting impaired cardiometabolic and renal function originating from HDP may increase the subsequent risk. A combination of these two mechanisms has been postulated to contribute to the onset of CVD
Interpregnancy care: towards preventing recurrent HDP in subsequent pregnancies (Fig. 3)
Prevalence and risk factors of recurrent HDP
The recurrence rate of HDP varies according to ethnicity and region, yet a meta-analysis of 22 studies reported a recurrence rate of 20.7% (95% CI [20.4–20.9]) [50]. The recurrence rate also differs based on the type of HDP in the index pregnancy [51]. The subsequent risks of gestational hypertension and preeclampsia in women who have experienced gestational hypertension during their first pregnancy are 11.3% and 3.4%, respectively, while in those who have experienced preeclampsia during their first pregnancy these risks are estimated at 7.4% and 14.7%, respectively [51]. Furthermore, the risk of recurrence varies based on the severity and onset of the previous HDP [52]. The known risk factors for recurrent HDP in subsequent pregnancies include a history of HDP, maternal age ≥ 35 years, interpregnancy interval ≥ 6 years, increased interpregnancy weight change, delivery of small-for-gestational-age infant, diabetes mellitus, gestational diabetes mellitus, and social deprivation [51, 53].
Interpregnancy weight change
A meta-analysis in 2020 showed that the recurrence risk rises with an increase in interpregnancy weight change (odds ratio [OR] 1.37, 95% CI [1.21–1.53]), while the risk decreases when interpregnancy weight change reduces (0.87 [0.75–0.99]) [54]. Similarly, an interpregnancy body mass index (BMI) gain of > 1 unit (kg/m2) was associated with a higher risk of preeclampsia and HDP (adjusted OR 1.39 [1.14–1.65] and 1.44 [1.21–1.66], respectively) [55]. These findings suggest that changes in interpregnancy BMI contribute substantially to HDP recurrence and highlight the potential to reduce HDP recurrence rate through postpartum weight loss. Consequently, the ACOG recommends restoring BMI to the normal range of 18.5–24.9 kg/m2 by the subsequent pregnancy [13]. However, from a feasibility perspective, this recommendation presents some issues. For instance, assuming that a woman with a height of 160 cm and a BMI of 35 kg/m2 wishes to conceive within three years, the woman would need to lose 25.6 kg (8.5 kg/year) to return to the normal BMI range. In general, the postpartum period is a demanding period for child-rearing, and postpartum women cannot devote sufficient time to self-care. Moreover, prior studies including these recommendations have solely assessed the amount of weight/BMI changes, without considering the time frame of the pregnancy interval.
Annual BMI change as a novel index for assessment of recurrence risk of HDP
To address these challenges, we introduced a novel index, the annual BMI change (i.e., BMI change per year between the index and subsequent pregnancies), considering the time frame [56]. This index enables a more accurate evaluation of the risk of recurrent HDP [56]. If the annual BMI increases within 0.2–0.6 kg/m2/year by the subsequent pregnancy, the adjusted OR is 1.26 (0.45–3.53), 3.49 (1.03–11.82) for 0.6–1.0 kg/m2/year, and 4.11 (1.29–13.11) for ≥1.0 kg/m2/year, with 0–0.2 kg/m2/year as the reference for physiological increase per year. Based on these clinical data, we aim to develop a recurrence risk assessment tool to achieve postpartum weight management by setting feasible body weight goals in collaboration with patients and healthcare providers (unpublished data). In this context, weight management needs to align with Specific, Measurable, Achievable, Relevant, and Time-bound (SMART) goal-setting approaches to increase the chances of achievement [57]. First, the significance lies in allowing women to set their weight goals collaboratively with healthcare providers, rather than unilaterally by providers. Informed shared decision-making between women and healthcare providers is essential. Second, this assessment tool needs to be designed under specific timeframes and deadlines; therefore, it should include individual variations in effort, significance, and enthusiasm that contribute to the goal achievement, avoiding unrealistic goal-setting that could impede objective’s attainment (Fig. 4).
Lifestyle modifications
Although the need for interpregnancy care, including education regarding pregnancy complications in subsequent pregnancies and lifestyle modifications to mitigate such risks, has long been emphasized, postpartum lifestyle modifications that target exclusively women with a history of HDP have not been definitively established [9, 12, 14]. Evidence supporting the incorporation of various lifestyle interventions to reduce long-term CVD risk is also lacking.
Generally, lifestyle modifications are fundamental and include dietary interventions (e.g., reducing salt intake, incorporating vegetables and fruits into diet, and moderating consumption of cholesterol-rich foods), exercise therapies (≥150 minutes per week), maintaining optimal body weight, and smoking cessation for the prevention of future cerebro- and cardiovascular complications (Fig. 4) [14, 58, 59]. The Dietary Approaches to Stop Hypertension (DASH) diet is a dietary plan specifically designed for patients with hypertension [60]. Sufficient evidence has demonstrated that the DASH diet is effective in lowering blood pressure, managing weight, and reducing CVD risk, while its potential benefit could be speculated for women with a history of HDP [60]. Furthermore, sustaining breastfeeding is also pivotal for cardiovascular protection [13, 14]. According to a recent meta-analysis published in 2022, breastfeeding significantly reduced the risk of CVD (hazard ratio 0.89, 95% CI [0.83–0.95]), strokes (0.88 [0.79–0.99]), and cardiovascular-related mortality (0.83 [0.76–0.92]) [61]. Consequently, similar benefits can be anticipated through sustained breastfeeding in women with a history of HDP. Nonetheless, women with a history of HDP exhibit higher rates of early breastfeeding discontinuation than those exhibited by women without HDP [62].
Low-dose aspirin use during subsequent pregnancy
Evidence regarding the prevention of preeclampsia through low-dose aspirin has been sufficiently accumulated; the ACOG recommends low-dose aspirin prophylaxis (81 mg/day) at bedtime from 12 to 28 gestational weeks (optimally before 16 weeks) until delivery for women who are at a high risk for preeclampsia [63]. The ISSHP proposes aspirin (100–150 mg), preferably starting before 16 weeks of gestation and discontinuing at 36 weeks [2]. Low-dose aspirin selectively inhibits the synthesis of placental thromboxane A2 which promotes blood clotting and vasoconstriction, thereby, preventing excessive blood clotting and maintaining blood flow and placental function [64, 65]. Low-dose aspirin was significantly associated with a reduced risk of preterm preeclampsia (OR 0.38, 95% CI [0.20–0.74]) [66]. However, significant risk reduction was confined to the subgroup in which aspirin was initiated at ≤ 16 weeks of gestation. According to the administration time-dependent effect of low-dose aspirin on blood pressure, the blood pressure-lowering effect is reported when administered at bedtime but not upon awakening [67]. Several guidelines recommend the administration of low-dose aspirin at bedtime [2, 68].
The following precautions should be taken when prescribing low-dose aspirin in Japan: (1) low-dose aspirin prophylaxis after 28 weeks of gestation is contraindicated in Japan. Although aspirin administration after 28 weeks may lead to prolonged gestation, premature closure of the ductus arteriosus, suppression of uterine contractions, and increased bleeding at delivery according to the medication instructions in Japan, several systematic reviews have shown no increased risk of hemorrhagic complications, congenital anomalies, or adverse fetal or neonatal effects [63]; (2) low-dose aspirin prophylaxis is not covered by insurance; and (3) while the ACOG recommends the use of low-dose aspirin for a wide range of women with high-risk pregnancies (e.g., those with multiple pregnancy, diabetes mellitus, and kidney disease), JSHHP recommends aspirin only for women with a history of preeclampsia. Regarding the duration of low-dose aspirin administration, a recent randomized clinical trial demonstrated that discontinuation of aspirin at 24–28 weeks of gestation was not inferior to continuing aspirin until delivery in women at high risk of preeclampsia [69]. This suggests that continuous administration beyond 28 weeks of gestation may not always be necessary.
Postpartum care: towards mitigating future disease risk (Fig. 3)
Uninterrupted postpartum health care
Based on the long-term cohort studies, clinical guidelines across various nations have highlighted the significance of postpartum follow-up care for women with a history of HDP [3, 13, 19, 23, 70, 71]. However, standardized postpartum care programs have not yet been fully established. Recently, methodologies for addressing comprehensive follow-up care programs have been actively discussed [9, 16]. Khosla and colleagues have proposed a 5-step framework: Step 1 - Education to improve interdisciplinary awareness among providers, Step 2 - Continuous postpartum visits at 6–8 weeks postpartum and then annually until 50 years of age, Step 3 - Monitoring (blood pressure, biomarkers, and anthropometrics at clinic or home), Step 4 - CVD risk assessment (glucose, lipids, race, lifestyle factors, and anthropometrics), and Step 5 - Team-based approach to CVD risk reduction (Multidisciplinary approach; cardiologists, midwives, dietitians, lifestyle coaches, and public health nurses) [16].
Regarding the timeline of postpartum care, women are often disconnected from ongoing medical care after delivery and may not seek care again until midlife, and after the manifestation of CVD and metabolic diseases. The ACOG recommends an initial postpartum visit within three weeks, followed by a comprehensive visit by 12 weeks postpartum, and annual cardiovascular follow-up assessment thereafter [19]. Conversely, the American Stroke Association and European Society of Hypertension advocate annual risk assessments but do not specifically address the timing of immediate postpartum visits [72].
Nevertheless, evidence regarding whether such a comprehensive, long-term, multidisciplinary approach effectively reduces future CVD remains insufficient, and additional studies are warranted. Regarding primary prevention, the cost-effectiveness of such extensive care from the early postpartum period should be examined in comparison with that of care from midlife onwards.
Clinical trials for women who have experienced HDP to reduce future CVD risk
Several interventional trials have been conducted to reduce short-term cardiovascular risks in women who have experienced HDP [73]. The BP-PRESELF trial demonstrated that home blood pressure monitoring in women with preeclampsia or HELLP syndrome reduced diastolic blood pressure by 4.9 mmHg, with 80% less diagnosed cases of hypertension at the 1-year follow-up [74]. Self-management of blood pressure in women after HDP results in a persistent reduction in diastolic blood pressure of 7 mmHg at 3–4 years postpartum [75]. A randomized controlled trial with six months of enalapril treatment reported improvement in echocardiographic measurements related to cardiac remodeling and diastolic function in women with preterm preeclampsia [76]. However, there is a paucity of sufficiently powered randomized controlled trials in the early years after HDP to guide evidence-based cardiovascular risk reduction in affected women [73].
Assessment of CVD risk
The ACC/AHA recommends individualized assessments of anticipated CVD risk [43]. Preeclampsia is categorized as a “risk-enhancing” factor, necessitating discussion between healthcare practitioners and patients on future CVD risk and primary prevention [43]. Since there are no specific risk assessment tools for CVD designed exclusively during the postpartum period, healthcare providers can utilize existing assessment tools (e.g. Framingham Risk Score, Reynolds Risk Score, QRISK, and NORRISK2) in postpartum women [77,78,79,80]. Recently, Fraser et al., demonstrated that the predicted 10-year CVD risk in women with a history of preeclampsia was significantly higher than that in women with normotensive delivery; however, the differences in absolute risk were modest [81]. Therefore, the authors concluded that CVD risk assessment is not necessarily necessary for women with a history of pregnancy complications such as preeclampsia and preterm birth; however, these complications provide information to identify women who would benefit from primary prevention to reduce CVD risk in later life [81]. Multidisciplinary collaboration between obstetricians, cardiologists, nephrologists, primary care physicians, and other healthcare professionals can ensure comprehensive care and risk assessment for these individuals (Fig. 4).
Advantages of postpartum and interpregnancy care compared with preconception care
While women are often focused on caring for their children after delivery, to the point that they may neglect their own care and health, the postpartum period is an ideal and valuable opportunity to reflect on their health. There are some advantages of postpartum and interpregnancy care over preconception care before the initial pregnancy: (1) A targeted approach for the high-risk population is possible. As history of HDP is the strongest predictor of recurrent HDP (ORs 3.0–16.7), obstetric care providers can target the most high-risk women effectively [56, 82]. This targeted approach enhances efficiency and alleviates the burden on healthcare providers. (2) Adherence to interventions may improve. Patient motivation, attitude, awareness level, and understanding of necessary lifestyle modifications can play a significant role in improving adherence [83]. Women who have experienced HDP are more likely to remain motivated and avoid dropping out if appropriate patient education is provided. The Transtheoretical Model, also known as the Stages of Change model, is a framework used to understand and guide behavioral change processes [84]. This model identifies how individuals progress through different stages of change (precontemplation, contemplation, preparation, action, and maintenance) when modifying their behavior. While women who receive preconception care usually coincide with the stages from precontemplation to contemplation, women with a history of HDP may have already progressed from contemplation to preparation. By aligning interventions with their appropriate stages, healthcare providers can effectively facilitate and support sustained behavioral changes. (3) Timely intervention is possible. Currently, the most effective evidence-based intervention for preeclampsia prevention is the prophylactic use of low-dose aspirin [64]. Through effective postpartum education, women who have experienced preeclampsia are more likely to seek timely intervention with aspirin in subsequent pregnancies, without missing the window for prescription. These facets collectively emphasize the pivotal role and benefits of implementing postpartum and interpregnancy care strategies in women with a history of HDP.
Challenges and prospects for postpartum and interpregnancy care
Challenges and issues regarding postpartum and interpregnancy care
Postpartum and interpregnancy care, distinct from preconception care before the first pregnancy, faces the challenges of being applied to women who are often preoccupied with childcare, thereby limiting their ability to dedicate ample time to their own health. In addition, up to 40% of women do not attend postpartum visit in some countries [19]. Therefore, while an annual follow-up assessment is desirable, its feasibility remains challenging. However, in a recent report by Hirosaki University, in which a progressive approach to postpartum follow-up for women with a history of pregnancy complications was implemented, the 3-year follow-up rate was 78.8% [85].
Moreover, several questions need to be addressed regarding who should provide long-term postpartum care (obstetricians, primary care physicians, or routine medical checkups), whether the costs of screening for CVD are covered by insurance or self-funded, timing that healthcare providers should provide patient education for more effective outcomes (at diagnosis during pregnancy, between immediate delivery and discharge from hospital, or initial postpartum visit), and who and how to perform patient education (by doctor or nurse and by pamphlets, video, or individual counseling). However, the postpartum care system largely differs by country, health insurance system (public and private health insurance), coverage (insurance plan and provider), and human resources. Therefore, these questions need to be answered at a country, facility and physician level.
Women who need long-term postpartum assessment and interpregnancy care are not limited to those with a history of HDP but also include women who have experienced gestational diabetes mellitus, preterm birth, and other placental syndromes (e.g., fetal growth restrictions and placental abruption), which together account for 15–25% of all postpartum women [86,87,88]. Therefore, the issue of whether sufficient time can be allocated to achieve patient-centered postpartum care for high-risk women raises concerns from the viewpoint of human resources. Digital health technology may solve this problem and play a valuable role in enhancing patient education and facilitating the adoption of behaviors to achieve lifestyle modifications [89].
Increased awareness among patients and healthcare providers
According to a cross-sectional study conducted in Australia, individuals who are aware of their CVD risks following HDP are more likely to engage in health-seeking behaviors to reduce their risks [90]. Increased awareness through patient education may improve motivation, preventive efforts, and patient adherence (Fig. 4). Successful patient education that goes beyond the transfer of knowledge empowers patients to make informed decisions and take responsibility of their own health. The following strategies are acknowledged for successful patient education: a tailored approach, clear communication, use of visual aids and digital devices, repetition, multidisciplinary approach, empowerment, and feedback [91,92,93]. The methodology of patient education in women with a history of HDP requires further investigation.
However, challenges and concerns persist among obstetricians and gynecologists initiating patient education and primary care physicians responsible for providing long-term postpartum care. A substantial proportion of obstetricians and gynecologists are not thoroughly familiarized with the increased risk of recurrent HDP and subsequent CVD in women with a history of HDP, resulting in inadequate information provision for their patients.
Nevertheless, the clinical guidelines for obstetrical practice 2023 by the Japan Society of Obstetrics and Gynecology and the Japan Association of Obstetricians and Gynecologists incorporated information on future cardiovascular risks among women with a history of HDP for the first time (Clinical Question 309-2: Women with a diagnosis of HDP have an elevated risk of future hypertension, cerebrovascular and cardiovascular diseases, diabetes mellitus, and CKD. Therefore, regular long-term medical checkups are recommended.). This recommendation is expected to increase awareness of obstetricians and gynecologists and ensure appropriate information provision for women with a history of HDP (Fig. 4).
Internists and primary care physicians responsible for the long-term follow-up care of these women also require comprehensive knowledge of HDP. However, according to web-based panel surveys, only one in four clinical physicians accurately recognized the cardiovascular risks associated with HDP [94]. To develop a multidisciplinary support system for women with HDP, the JSSHP established a healthcare provider program in 2023. This program was designed for various healthcare providers, including obstetricians, internists, nurses, midwives, dietitians, pharmacists, and other healthcare professionals and aimed to develop expertise in HDP-related knowledge and practice specialized care through team-based approaches during the pre-pregnancy, pregnancy, and postpartum periods, to promote women’s overall health. Such initiatives hold the potential for the widespread adoption of postpartum and interpregnancy care for women with a history of HDP across various healthcare professionals disciplines through a multidisciplinary approach (Fig. 4).
Perspectives in Asia
It is well-known that the prevalence of CVD and metabolic diseases largely differs according to ethnicity. Therefore, further evidence on the Asian population is needed.
Conclusion
Women who have experienced HDP can become aware of future disease risk at a relatively young age, from their 20 s to early 40 s, therefore, they have a valuable opportunity to improve their lifestyle and undergo regular health checkups, thus mitigating CVD risk. From this perspective, pregnancy, which is considered a maternal stress test, provides with a valuable opportunity to identify women with risk factors for CVD and metabolic disease. This information should be provided to postpartum women and their families through counseling, while systematic health checks, and tailored lifestyle guidance should be implemented for those at high risk. Achieving effective postpartum care requires concerted efforts beyond the realms of obstetrics and gynecology, which means that collaboration with primary care physicians, internists (particularly in cardiology, nephrology, and endocrinology), nurse practitioners, and other healthcare providers is indispensable.
Moreover, within the domain of postpartum and interpregnancy care, numerous challenges and questions exist, underscoring the need for future research in this area. Although women with a history of HDP are inherently at a higher risk of CVD and metabolic syndrome, not all women with such a history are afflicted. The establishment of algorithms that can identify subsets of women at particularly higher risk and the exploration of early diagnostic biomarkers for potential therapeutic interventions are promising areas requiring further research.
References
Dimitriadis E, et al. Pre-eclampsia. Nat Rev Dis Prim. 2023;9:8.
Magee LA, et al. The 2021 International Society for the Study of Hypertension in Pregnancy classification, diagnosis & management recommendations for international practice. Pregnancy Hypertens. 2022;27:148–69.
Takagi K, et al. A Review of the Best Practice Guide 2021 for the Diagnosis and Management of Hypertensive Disorders of Pregnancy (HDP). Hypertens Res Pregnancy. 2022;10:57–73.
Chappell LC, et al. Pre-eclampsia. Lancet. 2021;398:341–54.
Say L, et al. Global causes of maternal death: a WHO systematic analysis. Lancet Glob Health. 2014;2:e323–e333.
Roberts CL, et al. Hypertensive disorders in pregnancy: a population-based study. Med J Aust. 2005;182:332–5.
Cameron NA, et al. Trends in the incidence of new‐onset hypertensive disorders of pregnancy among rural and urban areas in the United States, 2007 to 2019. J Am Heart Assoc. 2022;11:e023791.
Ford ND, et al. Hypertensive disorders in pregnancy and mortality at delivery hospitalization - United States, 2017-2019. MMWR Morb Mortal Wkly Rep. 2022;71:585–91.
Hauspurg A, Countouris ME, Catov JM. Hypertensive disorders of pregnancy and future maternal health: how can the evidence guide postpartum management? Curr Hypertens Rep. 2019;21:96.
Ditisheim A, et al. Prevalence of hypertensive phenotypes after Preeclampsia. Hypertension. 2018;71:103–9.
Giorgione V, et al. Incidence of postpartum hypertension within 2 years of a pregnancy complicated by pre-eclampsia: a systematic review and meta-analysis. Int J Obstet Gynaecol. 2021;128:495–503.
Poon LC, et al. Hypertensive disorders of pregnancy and long-term cardiovascular health: FIGO Best Practice Advice. Int J Gynecol Obstet. 2023;160:22–34.
Obstetric Care Consensus No. 8. Interpregnancy Care. Obstet Gynecol. 2019;133:e51–e72.
Khan SS, et al. Optimizing prepregnancy cardiovascular health to improve outcomes in pregnant and postpartum individuals and offspring: a scientific statement from the American Heart Association. Circulation. 2023;147:e76–e91.
Ogunwole SM, et al. Interconception care for primary care providers: consensus recommendations on preconception and postpartum management of reproductive-age patients with medical comorbidities. Mayo Clin Proc Innov Qual Outcomes. 2021;5:872–90.
Khosla K, et al. Long-term cardiovascular disease risk in women after hypertensive disorders of pregnancy: recent advances in hypertension. Hypertension. 2021;78:927–35.
Berks D, et al. Feasibility and effectiveness of a lifestyle intervention after complicated pregnancies to improve risk factors for future cardiometabolic disease. Pregnancy Hypertens. 2019;15:98–107.
WHO. Meeting to develop a global consensus on preconception care to reduce maternal and childhood mortality and morbidity. World Health Organization Headquarters, Geneva, 6–7 February 2012: meeting report.
ACOG Committee Opinion No. 736. Optimizing postpartum care. Obstet Gynecol. 2018;131:e140–e150.
İnce, S and NY Albar, Physiological Changes During the Postpartum Period: General Overview, in ENT Diseases: Diagnosis and Treatment during Pregnancy and Lactation, C Cingi, HE Özel, and N Bayar Muluk, Editors. 2022, Springer International Publishing: Cham. p. 29–38.
Ushida T, et al. New-onset postpartum hypertension in women without a history of hypertensive disorders of pregnancy: a multicenter study in Japan. Hypertens Res. 2023;46:2583–92.
Gestational Hypertension and Preeclampsia. ACOG Practice Bulletin, Number 222. Obstet Gynecol. 2020;135:e237–e260.
Webster K, et al. Diagnosis and management of hypertension in pregnancy: summary of updated NICE guidance. Bmj. 2019;366:l5119.
Tanaka H, et al. Are there maternal deaths related to hemorrhagic stroke due to hypertensive disorder of pregnancy that could be potentially preventable by tight hypertension management in antepartum? A retrospective study from the Maternal Death Exploratory Committee in Japan. J Clin Med. 2023;12:2908.
Norwitz ER. Preeclampsia: Intrapartum and postpartum management and long-term prognosis. Post TW, editor. UpToDate. Waltham, MA; UpToDate Inc. http://www.uptodate.com (Accessed on Feb 22, 2024).
Petersen EE, et al. Vital signs: pregnancy-related deaths, United States, 2011–2015, and strategies for prevention, 13 States, 2013-2017. MMWR Morb Mortal Wkly Rep. 2019;68:423–9.
Katsuragi S, et al. Analysis of preventability of hypertensive disorder in pregnancy-related maternal death using the nationwide registration system of maternal deaths in Japan. J Matern Fetal Neonatal Med. 2019;32:3420–6.
Sibai BM, et al. Maternal morbidity and mortality in 442 pregnancies with hemolysis, elevated liver enzymes, and low platelets (HELLP syndrome). Am J Obstet Gynecol. 1993;169:1000–6.
Japanese Society of Nephrology. Essential points from Evidence-based Clinical Practice Guidelines for Chronic Kidney Disease 2018. Clin Exp Nephrol. 2019;23:1–15.
Wu P, et al. Preeclampsia and future cardiovascular health. Circulation: Cardiovasc Qual Outcomes. 2017;10:e003497.
Dall’Asta A, et al. Cardiovascular events following pregnancy complicated by pre-eclampsia with emphasis on comparison between early- and late-onset forms: systematic review and meta-analysis. Ultrasound Obstet Gynecol. 2021;57:698–709.
Mito A, et al. Hypertensive disorders of pregnancy: a strong risk factor for subsequent hypertension 5 years after delivery. Hypertens Res. 2018;41:141–6.
Oishi M, et al. Hypertensive disorders of pregnancy increase the risk for chronic kidney disease: A population-based retrospective study. Clin Exp Hypertens. 2017;39:361–5.
Riise HKR, et al. Incident coronary heart disease after preeclampsia: role of reduced fetal growth, preterm delivery, and parity. J Am Heart Assoc. 2017;6:e004158.
Theilen LH, et al. Long-term mortality risk and life expectancy following recurrent hypertensive disease of pregnancy. Am J Obstet Gynecol. 2018;219:107.e1–107.e6.
Honigberg MC, et al. Heart failure in women with hypertensive disorders of pregnancy. Hypertension. 2020;76:1506–13.
Leon LJ, et al. Preeclampsia and cardiovascular disease in a large UK pregnancy cohort of linked electronic health records: A CALIBER study. Circulation. 2019;140:1050–60.
Adank MC, et al. Hypertensive disorders of pregnancy and cognitive impairment: a prospective cohort study. Neurology. 2021;96:e709–e718.
Schliep KC, et al. Association between hypertensive disorders of pregnancy and dementia: a systematic review and meta-analysis. Hypertension. 2023;80:257–67.
Dayan N, et al. Impact of preeclampsia on long-term cognitive function. Hypertension. 2018;72:1374–80.
Romundstad PR, et al. Hypertension in pregnancy and later cardiovascular risk: common antecedents? Circulation. 2010;122:579–84.
Umemura S, et al. The Japanese Society of Hypertension Guidelines for the Management of Hypertension (JSH 2019). Hypertens Res. 2019;42:1235–481.
Arnett DK, et al. 2019 ACC/AHA Guideline on the Primary Prevention of Cardiovascular Disease: A Report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines. Circulation. 2019;140:e596–e646.
Bartsch E, et al. Clinical risk factors for pre-eclampsia determined in early pregnancy: systematic review and meta-analysis of large cohort studies. BMJ. 2016;353:i1753.
Sanghavi M, Rutherford JD. Cardiovascular physiology of pregnancy. Circulation. 2014;130:1003–8.
Sattar N, Greer IA. Pregnancy complications and maternal cardiovascular risk: opportunities for intervention and screening? BMJ. 2002;325:157–60.
Pruthi D, et al. Exposure to experimental preeclampsia in mice enhances the vascular response to future injury. Hypertension. 2015;65:863–70.
Ushida T, et al. Persistence of risk factors associated with maternal cardiovascular disease following aberrant inflammation in rat pregnancy. Biol Reprod. 2017;97:143–52.
Ushida T, et al. Postpartum alterations following inflammation in rat pregnancy: a discovery proteomic analysis. Reproduction. 2021;161:513–22.
van Oostwaard MF, et al. Recurrence of hypertensive disorders of pregnancy: an individual patient data meta-analysis. Am J Obstet Gynecol. 2015;212:624.e1–17.
Lailler G, et al. Recurrence of hypertensive disorders of pregnancy: results from a nationwide prospective cohort study (CONCEPTION). BJOG: Int J Obstet Gynaecol. 2023;130:902–12.
Barton JR, Sibai BM. Prediction and prevention of recurrent preeclampsia. Obstet Gynecol. 2008;112:359–72.
Ebbing C, et al. Risk factors for recurrence of hypertensive disorders of pregnancy, a population-based cohort study. Acta Obstet Gynecol Scand. 2017;96:243–50.
Martínez-Hortelano JA, et al. Interpregnancy weight change and hypertension during pregnancy: a systematic review and meta-analysis. Obstet Gynecol. 2020;135:68–79.
Teulings NEWD, et al. Effect of interpregnancy weight change on perinatal outcomes: systematic review and meta-analysis. BMC Pregnancy Childbirth. 2019;19:386.
Tano S, et al. Annual body mass index gain and risk of hypertensive disorders of pregnancy in a subsequent pregnancy. Sci Rep. 2021;11:22519.
Doran GT. There’s a S.M.A.R.T. way to write managements’s goals and objectives. Manag Rev. 1981;70:35–36.
Rippe JM. Lifestyle strategies for risk factor reduction, prevention, and treatment of cardiovascular disease. Am J Lifestyle Med. 2019;13:204–12.
van Trier TJ, et al. Lifestyle management to prevent atherosclerotic cardiovascular disease: evidence and challenges. Neth Heart J. 2022;30:3–14.
Moore TJ, et al. DASH (Dietary Approaches to Stop Hypertension) diet is effective treatment for stage 1 isolated systolic hypertension. Hypertension. 2001;38:155–8.
Tschiderer L, et al. Breastfeeding is associated with a reduced maternal cardiovascular risk: systematic review and meta-analysis involving data from 8 studies and 1 192 700 Parous women. J Am Heart Assoc. 2022;11:e022746.
Burgess A, Eichelman E, Rhodes B. Lactation patterns in women with hypertensive disorders of pregnancy: an analysis of Illinois 2012–2015 Pregnancy Risk Assessment Monitoring System (PRAMS) Data. Matern Child Health J. 2021;25:666–75.
ACOG Committee Opinion No. 743. Low-dose aspirin use during pregnancy. Obstet Gynecol. 2018;132:e44–e52.
Roberge S, Bujold E, Nicolaides KH. Aspirin for the prevention of preterm and term preeclampsia: systematic review and metaanalysis. Am J Obstet Gynecol. 2018;218:287–293.e1.
Ren Y, et al. Application of low dose aspirin in pre-eclampsia. Front Med. 2023;10:1111371.
Rolnik DL, et al. Aspirin versus Placebo in pregnancies at high risk for preterm preeclampsia. N. Engl J Med. 2017;377:613–622.
Hermida RC, et al. Aspirin administered at bedtime, but not on awakening, has an effect on ambulatory blood pressure in hypertensive patients. J Am Coll Cardiol. 2005;46:975–83.
Stefanovic V. International Academy of Perinatal Medicine (IAPM) Guidelines for Screening, Prediction, Prevention and Management of Pre-eclampsia to Reduce Maternal Mortality in Developing Countries. J Perinat Med. 2023;51:164–9.
Mendoza M, et al. Aspirin discontinuation at 24 to 28 weeks’ gestation in pregnancies at high risk of preterm preeclampsia: a randomized clinical trial. Jama. 2023;329:542–50.
Brown MA, et al. Hypertensive disorders of pregnancy: ISSHP classification, diagnosis, and management recommendations for international practice. Hypertension. 2018;72:24–43.
Carver AR, et al. Maternal pravastatin prevents altered fetal brain development in a preeclamptic CD-1 mouse model. PLoS One. 2014;9:e100873.
Regitz-Zagrosek V, et al. 2018 ESC Guidelines for the management of cardiovascular diseases during pregnancy: The Task Force for the Management of Cardiovascular Diseases during Pregnancy of the European Society of Cardiology (ESC). Eur Heart J. 2018;39:3165–241.
Lui NA, Jeyaram G, Henry A. Postpartum interventions to reduce long-term cardiovascular disease risk in women after hypertensive disorders of pregnancy: a systematic review. Front Cardiovasc Med. 2019;6:160.
Muijsers HEC, et al. Home blood pressure monitoring detects unrevealed hypertension in women with a history of preeclampsia: Results of the BP-PRESELF study. Am. J Prev Cardiol. 2022;12:100429.
Kitt JA, et al. Short-term postpartum blood pressure self-management and long-term blood pressure control: a randomized controlled trial. Hypertension. 2021;78:469–79.
Ormesher L, et al. Postnatal Enalapril to Improve Cardiovascular Function Following Preterm Preeclampsia (PICk-UP):: A Randomized Double-Blind Placebo-Controlled Feasibility Trial. Hypertension. 2020;76:1828–37.
Wilson PW, et al. Prediction of coronary heart disease using risk factor categories. Circulation. 1998;97:1837–47.
Ridker PM, et al. Development and validation of improved algorithms for the assessment of global cardiovascular risk in women: the Reynolds Risk Score. Jama. 2007;297:611–9.
Hippisley-Cox J, et al. Derivation and validation of QRISK, a new cardiovascular disease risk score for the United Kingdom: prospective open cohort study. BMJ. 2007;335:136.
Selmer R, et al. NORRISK 2: A Norwegian risk model for acute cerebral stroke and myocardial infarction. Eur J Prev Cardiol. 2017;24:773–82.
Fraser A, et al. Ten‐year cardiovascular disease risk trajectories by obstetric history: a longitudinal study in the Norwegian HUNT Study. J Am Heart Assoc. 2022;11:e021733.
Zhang J, Troendle JF, Levine RJ. Risks of hypertensive disorders in the second pregnancy. Paediatr Perinat Epidemiol. 2001;15:226–31.
World Health, O., Adherence to long-term therapies : evidence for action. 2003, World Health Organization: Geneva.
Prochaska JO, DiClemente CC. Stages and processes of self-change of smoking: toward an integrative model of change. J Consult Clin Psychol. 1983;51:390–5.
Oishi M, et al. Current status of long-term follow-up system for women with a history of hypertensive disorders of pregnancy: the HDP-PPAP study (HDP-Postpartum in Aomori prefecture study). J Matern Fetal Neonatal Med. 2023;36:2183757.
Fraser A, Catov JM. Placental syndromes and long-term risk of hypertension. J Hum Hypertens. 2023;37:671–4.
Ananth CV, et al. Maternal cardiovascular and cerebrovascular health after placental abruption: a systematic review and meta-analysis (CHAP-SR). Am J Epidemiol. 2021;190:2718–29.
Green JB. Cardiovascular consequences of gestational diabetes. Circulation. 2021;143:988–90.
Kuwabara A, Su S, Krauss J. Utilizing digital health technologies for patient education in lifestyle medicine. Am J Lifestyle Med. 2020;14:137–42.
Atkinson J, et al. Patients’ understanding of long-term cardiovascular risks and associated health-seeking behaviours after pre-eclampsia. Open Heart. 2023;10:e002230.
Wang M, et al. Perceptions of patients and healthcare providers on patient education to improve oral anticoagulant management. J Eval Clin Pract. 2022;28:1027–36.
Timmers T, et al. Educating patients by providing timely information using smartphone and tablet apps: systematic review. J Med Internet Res. 2020;22:e17342.
Ndosi M, et al. Effects of needs-based patient education on self-efficacy and health outcomes in people with rheumatoid arthritis: a multicentre, single blind, randomised controlled trial. Ann Rheum Dis. 2016;75:1126–32.
Ford ND, et al. Clinician knowledge and practices related to a patient history of hypertensive disorders of pregnancy. Obstet Gynecol. 2022;139:898–906.
Acknowledgements
The authors thank Editage (www.editage.jp) for the English language editing.
Funding
This study was supported by grants awarded to TU by the Japan Society for the Promotion of Science (JSPS KAKENHI 22K16857) and Yamaguchi Endocrine Research Foundation.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Ushida, T., Tano, S., Imai, K. et al. Postpartum and interpregnancy care of women with a history of hypertensive disorders of pregnancy. Hypertens Res 47, 1457–1469 (2024). https://doi.org/10.1038/s41440-024-01641-7
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41440-024-01641-7
Keywords
This article is cited by
-
Consider hypertension risk factors once again
Hypertension Research (2024)